|
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|
CLINICAL STUDIES / ETUDES CLINIQUES
RISK FACTORS FOR EPILEPSY IN CHILDREN WITH CEREBRAL PALSY
FACTEURS DE RISQUE DANS L'EPILEPSIE AVEC PARALYSIE CÉRÉBRALE
E-Mail Contact - LAGUNJU IkeOluwa Abiola :
ilagunju@yahoo.co.uk
ABSTRACT Background Objectives Methods Results Conclusion Key words: Africa,Epilepsy, risk factors, cerebral palsy RESUME Introduction Méthode Résultat Conclusion Mots clefs : Afrique, épilepsie, facteurs de risque, paralysie cérébrale. INTRODUCTION Cerebral palsy (CP) refers to a group of non-progressive, but often changing motor impairment syndromes secondary to lesions or anomalies of the brain arising in the early stages of development.[14] It is a major cause of disability in childhood,[1,17] and has been described as one of the three most common life-long developmental disabilities, the other two being autism and mental retardation.[22] The incidence of cerebral palsy in the developed world is about 2 – 2.5/1,000 live births.[18,20] This has remained largely unchanged despite advances in obstetric care and has been partly attributed to the increased survival of preterm infants.[16] Epilepsy refers to recurrent afebrile seizures and has been reported to occur in about 1% of the population.[7,25] A much higher incidence is however seen in children with cerebral palsy and about 15-90% of children with cerebral palsy have been reported to suffer from epilepsy.[5,10,23] Common forms of seizures and epilepsy syndromes reported in children with cerebral palsy in literature include generalized tonic clonic seizures, partial seizures, infantile spasms, myoclonic epilepsy and Lennox Gastaut syndrome.[5,10,23] In a developing country setting, epilepsy poses additional economic and psychological stress with considerable hardship on the affected children and their families. This study sets out to describe the risk factors for epilepsy in children with cerebral palsy seen at the University College Hospital, Ibadan. The findings in this study will aid early diagnosis and prompt management of epilepsy in children with cerebral palsy. MATERIAL AND METHODS The study was a cross sectional study carried out over a period of two years. All cases of cerebral palsy seen at the Paediatric Neurology clinic, University College Hospital, Ibadan, Nigeria between June 2003 and May 2005 were studied. The diagnosis of cerebral palsy was clinical, based on a history of abnormal motor development that was not progressive, coupled with the presence of abnormal neurological signs that localized the lesion to the brain. [21] All the diagnoses were made by the Paediatric Neurologist(s) and all the children who satisfied the diagnostic criteria were enrolled into the study. Epilepsy was defined as separate occurrence of two or more unprovoked seizures, not diagnosed as neonatal or febrile seizures. [9] The diagnosis of epilepsy was based on history from a reliable eye witness account and EEG findings. Spasticity involving one upper limb and the ipsilateral lower limb was classified as hemiplegia, spasticity of all four limbs, with the upper limb involvement more marked than or equal to that of the lower limbs- spastic quadriplegia, spasticity of the lower extremities, with a variable but lesser involvement of the upper limbs, spastic diplegia. Cases with extra pyramidal symptoms were classified as dyskinetic, those with hypotonia classified as hypotonic, while the mixed class had a combination of features of the spastic and extrapyramidal types.[10] Informed consent was obtained from the care-givers of all the subjects. A detailed history of the illness, development, pregnancy, birth and neonatal periods were taken at presentation. A thorough neurologic examination was carried out on each patient at presentation and this entailed assessment of consciousness, speech, cranial nerves, cerebellar, motor and sensory functions. All the patients with epilepsy had electroencephalography done and the findings were recorded. Cranial computerized tomography scan was performed in 20 cases and this included all the cases of congenital malformations of the brain and suspected intrauterine infections. The high cost of this investigation made it unaffordable to most of the patients. The following information was obtained on each patient: sociodemographic data, age at first presentation, history of neonatal seizures, gestational age at and place of delivery. The underlying cause of CP, and the appropriate physiologic and topographic classes were also recorded in each patient. All the children were referred to the Ophthalmologists, Audiologist and Clinical psychologists for visual, hearing and intelligent quotient (IQ) assessment respectively. Additional information obtained in those with epilepsy included: age at first seizure, type of seizure and findings on electroencephalography. RESULTS A total of one hundred and seventy six children with cerebral palsy were seen at the Paediatric Neurology clinic of the University College Hospital, Ibadan, Nigeria during the period of study. There were 110 males and 66 females, giving a male to female ratio of 1.7:1. The mean age of the children was 28.4 (SD=28.6) months and about two-thirds of them were below the age of 2 years. The mean age at diagnosis of cerebral palsy was 18.3 months (SD=14.5) months. The most frequent underlying causes of cerebral palsy in the study were severe birth asphyxia (46.3%), severe neonatal jaundice (25.4%) and post infectious brain damage (10.2%). Prematurity, intrauterine infections, congenital malformations of the brain and trauma accounted for a total of 13.6% while the aetiology of cerebral palsy could not be ascertained in 4.0% cases. Spastic form of cerebral palsy was the most prevalent in the study, found in 83.5% cases. Other forms of CP seen were mixed (7.6%), dyskinetic (6.5%) and hypotonic (2.4%). Sixty five (36.9%) of the cases had associated epilepsy. The frequency of epilepsy was highest in children with spastic hemiplegia (50%) and spastic quadriplegia (40%). Children with spastic diplegia and dyskinetic CP had epilepsy prevalence rates of 20% and 16.6% respectively while none of the three children with spastic triplegia had associated epilepsy. The major seizure types were generalized tonic clonic seizures (53.8%), partial seizures (18.5%) and infantile spasms (15.4%). Other less common forms of epilepsy were myoclonic seizures (9.2%) and Lennox Gastaut syndrome (3.1%). The severe forms of epilepsy, namely infantile spasms and Lennox Gastaut syndrome were mainly seen in children with spastic quadriplegia while partial seizures were more frequently seen in those with spastic hemiplegia. Figure 1 shows the distribution of the seizure types in the topographic classes of CP. The median age at first seizure was 13.0 months. Figure 2 is a box plot showing the distribution of age at first seizure in the different topographic classes of cerebral palsy. Children with hemiplegic cerebral palsy developed epilepsy at a relatively older age when compared with spastic quadriplegia and diplegia. Forty nine (75.3%) of all the children with epilepsy had their first seizure in the first year of life; 86% of those with spastic quadriplegia developed epilepsy in the first year of life, while less than half (45%) of the hemiplegic group developed epilepsy in the first year of life (p= 0.002). A history of neonatal seizures was obtained in 29 (44.6%) of the children with CP and epilepsy. The relationship between epilepsy and patient’s characteristics is shown in table 1.Aetiology of cerebral palsy was significantly related to epilepsy (p=0.000) with patients who developed CP following post infectious brain damage having the highest proportions of epilepsy cases (73.7%) compared with birth asphyxia and neonatal jaundice. Seizures in the first year of life remained significant after adjusting for other variables with children with seizures over forty five times more likely to develop epilepsy than children free of seizures in the first year of life. Patients with the hemiplegic variety were about five times more likely than the remainder to suffer epilepsy and this was another significant predictor. (p=0.014) DISCUSSION Cerebral palsy remains a major cause of disability in childhood and in Ibadan, Nigeria, it is the second leading paediatric neurological disorder seen at the paediatric neurology clinic of the University College Hospital, Ibadan. [12] Sixty five of the children with cerebral palsy in this study had associated epilepsy, giving a prevalence rate of 36.9%. This finding is consistent with reports from other parts of the world; Kulak and Sobaniec[10] reported a prevalence of 41.4% in Poland while Carlson et al[5] found a prevalence rate of 38% among Swedish children with cerebral palsy. Higher values have however been reported in literature and this has been related to the greater severity of CP in the patients studied. Cerebral palsy thus remains a major risk factor for the development of epilepsy in childhood. The most common forms of seizure found in children with cerebral palsy in the study were generalized tonic clonic seizures (53.8), partial seizures (18.5%) and infantile spasms (15.4%). Other less common forms seen were myoclonic seizures and Lennox Gastaut syndrome. This finding is consistent with reports from previous studies.[7,11] Infantile spasms and Lennox Gastaut syndrome are severe forms of epilepsy which are seen more frequently in infants and children with underlying structural abnormalities of the brain. However, any of the various recognized seizure types can occur in cerebral palsy. The study showed a relationship between the aetiology of cerebral palsy and the risk of associated epilepsy. Children who developed cerebral palsy as a complication of intracranial infections had a significantly increased risk of epilepsy. Meningitis is the leading childhood intracranial infection seen in the developing world, Nigeria inclusive. The availability of effective vaccines has brought a dramatic decline in the incidence of meningitis and its attendant complications in the developed world. The findings in this study suggest that effective childhood immunization will bring a significant decline in the proportion of cerebral palsy and childhood epilepsies. Although, neurocognitive impairment has been shown to be frequent in individuals with epilepsy, [24] this study did not show any significant association between the presence of mental retardation and the development of epilepsy in children with CP. Presence of spastic hemiplegia was also found to be an important predictor of epilepsy in cerebral palsy. Epilepsy is known to be most common among the hemiplegic and quadriplegic forms of cerebral palsy. [10,11] The study showed that children with hemiplegic cerebral palsy are about 5 times more likely than others to develop epilepsy (OR=5.18). This study identifies seizures in the first year of life and presence of spastic hemiplegia as major risk factors for the development of epilepsy in children with cerebral palsy. Identification of these risk factors will aid early diagnosis and prompt institution of anti-epileptic drug therapy in children with cerebral palsy. CONCLUSION Epilepsy is a frequent problem in children with cerebral palsy. A history of neonatal seizures, occurrence of seizures in the first year of life, presence of spastic hemiplegia and post infectious brain damage all warrant a close evaluation and appropriate follow up for early detection of epilepsy in children with cerebral palsy.
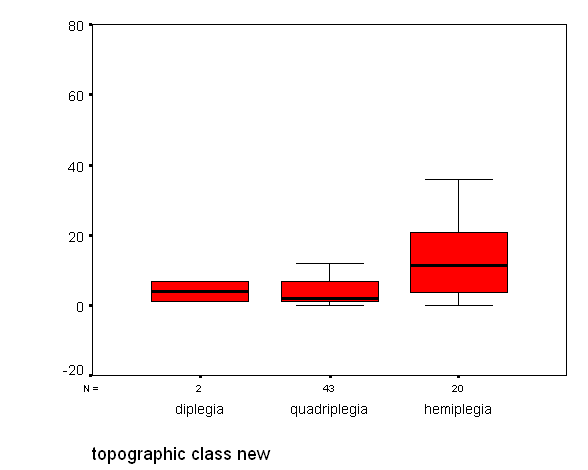
Fig 2. Box plot showing the distribution of age at first seizure in the topographic classes of cerebral palsy in children with CP and epilepsy Table 1: Characteristics of patients with Cerebral Palsy (CP) and Epilepsy and CP without Epilepsy
Table 2: Bivariate associations between epilepsy and predictor variables
Table 3: Logistic regression analysis of epilepsy on predictor variables
REFERENCES
|
© 2002-2018 African Journal of Neurological Sciences.
All rights reserved. Terms of use.
Tous droits réservés. Termes d'Utilisation.
ISSN: 1992-2647