|
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|
NEUROEPIDEMIOLOGY
PROFILE OF STROKE IN NIGERIANS: A PROSPECTIVE CLINICAL STUDY
PROFIL DES ACCIDENTS VASCULAIRES CEREBRAUX AU NIGERIA : UNE ETUDE PROSPECTIVE
E-Mail Contact - KOMOLAFE Morenikeji Adeyoyin :
adeyoyin2001@yahoo.com
ABSTRACT Background and purpose Methods Results Conclusion Key words: Stroke, Clinical profile, computerized tomography scan, Nigerians. RESUME Introduction Objectifs Méthodes Résultats Conclusions Mots Cles : Accident vasculaire cérébral, Afrique, Epidémiologie, Hypertension artérielle, Nigéria, Scanner INTRODUCTION Stroke, defined by the World Health Organization as “rapidly developing signs of focal or global disturbance of cerebral or intracranial neuronal function with symptoms lasting for more than 24 hours or leading to the death of the patient with no apparent cause other than that of vascular origin”17 is a major cause of death worldwide, second only to ischaemic heart disease8. Stroke is the leading cause of neurological disability in adults5, 18. Stroke is also a leading cause of morbidity and mortality in adults in the productive ages that contribute the work force of the society6. The hospital frequency of stroke at the University College Hospital Ibadan in 1969 was between 0.9 and 46% of all hospital admissions and 41% of all neurological admissions10. There appears to be an increase in the hospital frequency of stroke as a recent review at the University College Hospital Ibadan, 30 years later showed that stroke is now the leading cause of adult neurological admissions16. Stroke is increasingly becoming a major cause of morbidity and mortality in Nigeria and other developing countries19. Stroke has thus become a major public health problem in Nigeria. Stroke patients suffer from post stroke depression, a complication which occurs in 30% of cases19 and is associated with increase in morbidity and reduced survival14, 3. Apart from the burden of stroke on the survivors, those who care for them are also prone to emotional distress and a reduced quality of life. In a recent study at out center, the primary care givers of stroke patients were observed with higher rates of anxiety and depression and a lower quality of life when compared with matched controls2. With the increasing availability of computerized tomography scanners (CT scan) in most facilities including ours, the stroke sub-type can now be more accurately determined. The need to do CT scan was further highlighted in a study by Ogun et al7 in which the accuracy of clinical assessment was about 70% even in tertiary centers with many neurologists. The major risk factors for stroke in Nigerians are hypertension, diabetes, and hyperlipidaemia10. Cerebral infarction is the most common type of stroke seen occurring in 48% of patients while intracerebral haemorrhage occurs in 15.7% of patients and subarachnoid haemorrhage in 11.3% of patients11, 1. The mortality and severity of stroke is on the decline in developed countries because of life style modification, increased use of preventive measures such as adequate blood pressure control, increased use of anti- lipid drugs and aspirin15. This is in contrast to the increasing hospital frequency noted in our environment thus having a great burden on the health facilities in Nigerian hospitals. PATIENTS AND METHODS The study was a prospective hospital based study conducted at our centre which is a referral centre for about six out of the thirty-six states in the country. All the patients with diagnosis of stroke presenting to the Neurology unit of the Obafemi Awolowo University Teaching Hospitals Complex, Ile- Ife over a six year period (2000 to 2005) were consecutively recruited. Stroke was diagnosed using both clinical criteria and brain CT scan findings. RESULTS One hundred and thirty five stroke patients were managed during the 6-year study period. Stroke was responsible for 2.9% (135/4583) of all medical admissions and 22% (135/615) of all neurological admissions in our centre. The major predisposing factors noted were hypertension, diabetes mellitus and heart disease (atrial fibrillation) accounting for 73%, 16% and 2% respectively. Over half of the hypertensive patients (53.6%) were non-compliant with their drugs prior to the episode while 7% were previously unaware of their hypertensive status. The duration of symptoms before presentation ranged between 1 and 336 hours with a mean duration of 23 hours (SD 39). The duration of hospital admission ranged between one and 63 days with a mean of 10 days (SD 13). Stroke is undoubtedly an important disease worldwide and emerging as a public health problem in many nations. In our environment, the incidence of stroke in the community and the country is largely unknown since most studies in the country are hospital based. Even then a trend is seen as the hospital data shows progressive rise in the cases of stroke. Most authors believed that the hospital data is just a tip of the iceberg when compared to what may be seen in the community. Studies to determine the epidemiology of stroke in the community including the rural areas are therefore necessary to plan the prevention of stroke as well as manage the scarce resources in the treatment of the disease8. In this study, stroke accounted for about a quarter of the patients managed in the neurology unit of our centre during the six year period. In total, 135 patients that fulfilled the criteria were managed. The mean age was 62years (SD12) with a peak in the 5th and 6th decades of life (Table 1). This is in keeping with the findings of previous workers6, 11 where majority of the patients with stroke are in their fifth and sixth decades of life. We also noted a slight male preponderance (M:F = 1.3:1), also supporting findings in other studies and from community based studies16. Many studies showed that the male patient appear to have enhanced risk, especially for thrombotic strokes4. The higher prevalence of stroke in males might be due to the higher presence of cardiovascular risk factors in them. Also many of the males are in the upper social class and business men constantly exposed to stress and more likely to adopt a western type diet with consumption of refined, high cholesterol foods in combination with a sedentary lifestyle resulting in increased prevalence of cardiovascular risk factors such as hypertension, diabetes and hyperlipidaemia19. Our study like others in the country shows that thrombotic strokes were the most common11, 1. It is important to note that despite the availability of CT scan in our centre; only a third of the patients could afford the test. This clearly shows that cost is a major hindrance to the utilization of CT scan among stroke patients in Nigeria. This is a major problem that needs to be addressed as surgically treatable lesions such as glioma, meningioma, brain abscess and sub-dural haematoma could be mis-diagnosed as stroke in 8.6 to 13.5% of the cases3. At our centre, about twenty patients were excluded from the study as the CT scan showed surgically treatable lesions. This underscores the need for the attending physician to take a very good history of the events at onset of the stroke; however this may not be enough as it is sometimes difficult to differentiate medical from surgical conditions based on the clinical features alone without the aid of imaging modalities. The case of a 46year old long distance driver who slumped while taking his bath and hit his head aptly illustrates this point. He was being managed by the neurosurgical unit for head trauma and was to be taken for exploratory burr hole, when the relations were able to do a CT brain scan which showed massive intracerebral haemorrhage with intraventricular involvement Figure 2. All our patients save one were right handed, two-thirds of them had dominant hemispheric lesion with right hemiparesis. In a recent review of 450 cases in 20years by Onwuekwe et al9, their findings were similar to ours. The male to female ratio was 1.27:1 ant the mean age of their patients was 53.5yrs. They however found that their patients had almost equal distribution of right and left hemiparesis. They also found no significant difference between handedness and the sex of their patients. There were two cases of persistent vegetable state following cerebral infarction. One, a 48year-old woman (Figure 3a & 3b) with multiple infarcts had rapid reduction of her blood pressure at the secondary care center where she subsequently lapsed into coma prior to referral to our centre. This is a common practice by general practitioners with limited knowledge of the pathophysiology and treatment of stroke. Since majority of the patients will be attended to initially by this group of doctors, they need regular updates on the emergency care of stroke so as to improve the outcome of patients. Better still, they should be more actively involved in preventive programmes to detect risk factors and increase awareness generally. In conclusion, stroke is still a major problem in our environment and the major risk factor remains uncontrolled hypertension. The case fatality remains very high with a risk of moderate to severe neurological disability among the survivors. There is sub-optimal utilization of CT scan even when it is available because of financial constraints. We recommend that community based intervention measures such as health education of the community with emphasis on control of the predisposing factors, and education of general practitioners who are usually the first to handle stroke patients be put in place to address the burden of the problem and the inadequate control of blood pressure among hypertensive patients. The primary health workers should also be educated and trained to pass across information to the populace at every available opportunity the advantages of exercise, maintaining a healthy weight, avoid or quit smoking and monitoring of blood pressure and glucose levels regularly. There is also the need for pubic enlightenment campaigns to educate the populace about the need to check their blood pressures regularly and if hypertensive to comply with their medications. Efforts to make radiological imaging test available and affordable should be pursued both by the government and public institutions as well as by non governmental organisations. Table 1: Socio-demographic profile of stroke patients in Ile-Ife (N=135).
Table 2: Activity at onset of stroke patients in Ile-Ife (N= 135)
Others: During an argument (1), coming from night vigil (1), during defecation (1), during sexual intercourse (1), while preaching (2), while fetching water (1), while driving (2), and unknown (6). Table 3: Stroke outcome in Ile-Ife.
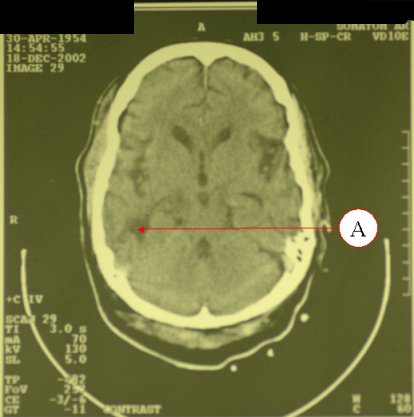
* 3 cases discharged against medical advice 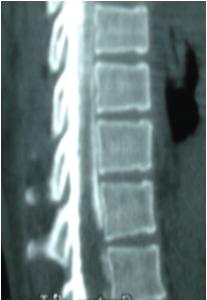 Figure 1
Figure 3a
REFERENCES
|
© 2002-2018 African Journal of Neurological Sciences.
All rights reserved. Terms of use.
Tous droits réservés. Termes d'Utilisation.
ISSN: 1992-2647