CLINICAL STUDIES / ETUDES CLINIQUES
HEADACHES IN CONSULTATION IN THE WORKPLACE IN OUAGADOUGOU (BURKINA FASO): IMPACT ON THE QUALITY OF LIFE AND THE PATIENT’S PROFESSIONAL PERFORMANCE
LES CEPHALEES EN CONSULTATION EN MILIEU DE TRAVAIL A OUAGADOUGOU (BURKINA FASO): IMPACT SUR LA QUALITE DE VIE ET LE RENDEMENT PROFESSIONNEL DES PATIENTS
- Service de Neurologie CHU de FANN, Dakar, Senegal
- Service de Neurologie, CHU Yalgado Ouédraogo, Ouagadougou, Burkina Faso
ABSTRACTS
Objective
Headaches are a real public health problem. This study describes the impact of headaches on quality of life and job performance in a working population in Ouagadougou.
Methods
This was a cross-sectional descriptive study from April to June 2011, conducted in six workplaces in the city of Ouagadougou and covering 110 workers. Workers with any headaches who consulted in health centers of workers during the study period were interested. The epidemiology, clinical aspect and impact of headaches were assessed using HIT-6 questionnaire and MIDAS test.
Results
The prevalence of headaches was estimated at 8%. The average age was 38.5 years old. By correlating the total number of workers in society by gender and the number of patient who consulted for headaches, we found 8% of females against 7% for males. Seen the profile of different companies, headaches were found mainly among laborers (67.3%). Following the history and clinical examination of patients, the prevalence of primary headaches was 83.6% against 16.4% for secondary headaches. Headaches with most significant impact on daily life were observed respectively for 17.3% and 31.8% in the HIT-6 test. Grade III and IV of disability were recorded respectively for 21.8% and 9.1% in the MIDAS test. The correlation between the functional disability associated with headaches and the professional category found moderate and severe disability respectively for 54.1% and 70% of laborers while no senior executive had moderate or severe functional disability. The correlation between the impact of headaches on the activities of daily life and the professional category found substantial and severe impact respectively for 78.9% and 57.2% of laborers while 5.7% of senior executives had a severe impact. the correlation between functional disability related to headaches and the gender found 10,5% of severe disability for women and 8.8% for men. The correlation between the impact of headaches on daily life and the gender found 42.1 of severe impact for women and 29.7% for men.
Conclusion
Headaches impose a heavy burden in the workplace especially for women and laborers. Their adequate care will improve the quality of life of workers with headaches for better work performance.
Keywords: Headaches, Impact, Quality of Life, Performance, Workplace, Burkina Faso
INTRODUCTION
Headaches are among the ten most frequent causes of consultation in the practice of general medicine [32]. This is a rather complex clinical symptom in its diagnostic and therapeutic approach [29], which puts headaches at the crossroads of medical disciplines [31]. The prevalence of headaches varies from 35% to almost 90% over a year in the general population [36].
Headaches have an impact on the quality of life of patients. They pose particular challenges for the working population and have a huge financial cost to society, mainly due to the loss of working hours and reduced productivity [25] that they are responsible. In the United Kingdom, for example, migraine alone is responsible for the loss of some 25 million days of work or school per year [25]. The tools for measuring their impact on quality of life are many, but the most used are the test MIDAS (Migraine Disability Assessment) and HIT-6 (Headache Impact Test) [37].
In recent years, in Africa, although many studies have been conducted on headaches, studies on the prevalence of headaches in the general population in Africa are few. Data collected in Zimbabwe from a study of the urban population had revealed a prevalence rate of 20.2% (17.6% for men and 27.0%) for women [4]. Despite the frequency of headaches, their social and economic impact, and current treatment options, no study to our knowledge has been conducted on the epidemiology, clinical aspects and impact of headaches on the quality of life and professional performance of patients with headaches in the city of Ouagadougou in Burkina Faso, which has motivated the realization of this work.
SUBJECTS AND METHODS
The study took place in Ouagadougou in Burkina Faso and the information were collected in six health centers of workers affiliated with the Regional Directorate of Health Workers at three separate areas. These were the Society of beverage distribution of Burkina Faso (SODIBO/BRAKINA) and the Society for metalworking and production of paints, adhesives, tiles (HAGE Industries) for Kossodo area; the cotton industry of Burkina Faso (FASO COTTON) and plastic processing Company of Burkina Faso (FASOPLAST) for Gounghin area; the National Lottery of Burkina Faso (LONAB) and the International Bank for Commerce, Industry, Agriculture of Burkina Faso (BICIAB) for LONAB area. These health centers of workers have been selected with agreement of Regional Directorate of Health centers of Workers of Burkina Faso because these companies have large numbers of employees and their health centers have more medical consultation.
This was a descriptive cross-sectional study over a period of 03 months, from 1st April 2011 to 30th June 2011 inclusive, which focused on workers with headaches, employee in each of the six listed companies, who consulted in one of health centers for headaches or any other disease with headaches and having suffered of headaches the three months before the interview. We were assisted for data collection by caregivers in different centers.
The study’s data were collected using a survey form, which included socio-demographic aspects (frequency, age, gender and occupation), clinical aspects (characters of headaches, triggers and the accompanying signs, patient history, clinical examination) and assessment of the impact of headaches on the performance and quality of life using the MIDAS test (Migraine Disability Assessment) and the HIT-6 questionnaire (Headache Impact Test). After the clinical examination, these tests were administered to each of patients with headaches. All types of headaches have been taken into account by these two scales.
To begin survey, we asked to each study participant his consent after we gave him or her information about objectives of this study. The identity of each participant kept confidential. Data were entered and analyzed using Epi Info in its version 3.5.1. The khi 2 test was used for statistical test at the 5% threshold.
RESULTS
1. Global results
The number and distribution of workers in the different companies are shown in Table I. The total numbers of consultations in the health centers of workers of each company during the 3 months of study and the number of consultations for headaches in these health centers during the same period are shown in Table II.
2. The socio-demographic characteristics
The average age of patients in consultation was 38.5 years old (yo). The youngest had 21 and the oldest, 59 yo. The age group of 30-39 yo was the most represented with thirty-six patients (32.7%). The males were most represented with 91 patients (82.7%) against 19 patients (17.3%) for the females. The prevalence of patients with headaches according to the distribution of the total of each company by gender is shown in Table III.
Laborers are the occupational category most observed in consultation for headaches with 74 patients (67.3%).
3. The clinical aspects
Hypertension was the most personal history found for 12 patients (10.9%) followed by the Ear, Nose and Throat (ENT) disorders (10.1%). Seventy-three (73) patients (66.4%) showed no particular history. Thirty-four (34) patients (30.9%) had diffuse headaches while 76 patients (69.1%) had localized headaches. Sixty-four (64) patients (58.2%) had pulsating headaches, 31 patients (28.2%) had tension headaches, 07 patients (6.4%) had headaches like heaviness, 05 patients (4.5%) had headaches like a constriction and 03 patients (2.7%) had headaches like electric discharge. Headaches occurred in daytime for 88 patients (80%) and in the night for 22 patients (20%).
Headaches had a paroxystic chronic evolution for 92 patients (83.6%) and recent onset for 18 patients (16.4%). The main triggering factors found were physical effort for 09 patients (8.2%) and a psychological factor for 08 patients (7.3%). Others patients no had specific triggers. Patients with headaches whose precipitating factor was related to physical effort incriminated particularly excessive workload (64.7%), work posture (17.7%), wearing heavy burden (17.6%). Patients with headaches whose precipitating factor was psychological have incriminated particularly stress related to their job (50%) and social and family problems in the same proportion of cases.
Concerning the accompanying signs, headaches with phonophobia were the most observed for 71 patients (64.5%), followed by headaches with vertigo (47.3%).
Physical examination found a systolic blood pressure (SBP) for the right arm of 122.1 ± 20.2 mmHg with extremes of 90 and 230 mmHg and for the left arm of 121.3 ± 19.6 mmHg with extremes of 80 and 210 mmHg. Diastolic blood pressure (DBP) average was for the right arm of 79.7 ± 14.1 mmHg with extremes of 70 and 140 mmHg and for the left arm of 79.5 ± 14 mmHg with extremes of 50 and 140 mmHg. The average temperature was 36.8°C ± 0.6. The lowest recorded was 35.3°C and the highest 38.7°C. The average heart and pulse rate were the same, 77.3 beats/min ± 10.7. The clinical examination of the nervous system was normal for all patients with headaches. The Cardiovascular signs consisted mainly of elevated blood pressure. Twelve (12) patients (10.9%) had a history of hypertension and 07 patients (6.4%) had high blood pressure found in the day exam. The ENT examination found that the main symptom associated with headaches was the hypertrophic rhinitis for 10 patients (9.1%).
According to the character of headaches, clinical examination and classification of the International Headache Society (IHS), 18 patients (16.4%) had headaches that started recently with the incriminated factor clearly identified. These were secondary headaches to a general affection for 14 patients and this factor was mainly hypertrophic rhinitis for 10 patients, tooth decay for 02 patients, a whitlow for 02 patients. Four (04) patients had headaches occurred after head injury. Eighty-two (92) patients (83.6%) had headaches with a chronic paroxysmal evolution with a normal clinical examination. These were primary headaches, classify into probable tension headaches for 65 patients (70.7%) and probable migraine for 27 patients (29.3 %).
4. The assessment of quality of life
The determination of the functional disability associated with headaches after using the MIDAS scale found:
– The average absenteeism in work because of headaches in the last three months preceding the examination of patients with headaches was less than 01 day (15.1h)
– The average of days during which the professional performance of patients with headaches was reduced by half or more in workplace because of headaches was 3.8 days
– The average of days during which, patients with headaches could not do their home work because of headaches was 2.3 days
– The average of days during which, patients with headaches reduced their domestic activity by half or more because of the headaches was 1.4 day
– The average days during which, patients with headaches had give up their family, social or recreational activities because of headaches is 1.1 day
The distribution of patients with headaches according to the four grades of increasing severity of functional disability is shown in Figure 1.
The distribution of patients with headaches according to the impact of headaches on their activities of daily life, evaluated with the HIT-6 questionnaire is shown in Figure 2.
By correlating the functional disability associated with headaches and the professional category, we observed that the functional disability was respectively moderate and severe for 13 (54.1%) and 7 (70%) laborers while no senior executive had moderate or severe functional disability.
By correlating the impact of headaches on the activities of daily life and the professional category, we found that the impact was substantial and severe respectively for 15 (78.9%) and 20 (57.2%) laborers while 2 (5.7%) senior executives had a severe impact.
By correlating the functional disability related to headaches and gender, females had the most severe disability with 10.5% against 08.8% for males.
By correlating the impact of headaches on daily life and gender, females had the impact most severe with 42.1% against 29.7% for males F.
DISCUSSION
The main restriction of the study was that no additional balance sheets like brain imaging were performed, limiting the diagnosis of secondary headaches.
1. The prevalence of headaches
Headaches are by far the most common neurological functional sign [03] and represent one of the most frequent reasons for consultation with the generalist or the neurologist [07, 09, 11, 14, 19, 26, 35]. Dousset estimates the prevalence of this sign to 90% in general [10]. Adoukonou, in a survey of headaches in enterprises in Cotonou, found a prevalence of 24.8% [1]. In our study in enterprises, on the 1395 patients in consultation, 110 (08%) had effectively headaches. This difference is undoubtedly related to the fact that we have included only patients who came themselves to consult for pain. During the study of Adoukonou, the choice of included patients in each company was made by a technique of systematic random sampling hence a much larger number of the study population. Also, in our study, according to the consultation register, it would seem for some companies employing seasonal workers like FASO COTTON, that these employees would be most prone to headaches. However, we haven’t been able to see them, saw the study period during which these seasonal workers were absent.
2. Socio-demographic aspects
2.1 Age
In our study, the mean age of patients was 38.5 years with extremes of 21 and 59 years. Adoukonou found an average age of 39.2 years in her study in Benin [1]. The age range of 30 to 39 years of patients with headaches was the most represented in our study (32.7%). Dravé in Burkina Faso and the Direction of Research, Studies, Evaluation and Statistics of France during the ten-yearly health survey (2002-2003), made the same observation by finding respectively 41.5% and 30% between 30 and 40 years [12, 28]. The age group of 50 to 59 was the least represented in our study, which is consistent with the literature, the prevalence of headaches decrease with age [13, 18, 28].
2.2. Gender
According to the literature, the prevalence of headaches was higher for women due to female preponderance of migraine and psychogenic headaches [6, 33]. In our study, headaches were observed among 91 men for 19 women. This is hardly surprising given the gender composition of the total of each of the companies. The prevalence of the patients men and women who consulted for headaches is however dependent on the distribution of the total of each companies by gender. Therefore, the correlation between the total number of women in companies and the number of women with headaches who consulted is significant and clearly established a dominance of headaches for women with 8% against 7% for men. This corroborates the data from literature on female preponderance of headaches [13, 27].
2.3. Professional category
Generally in our study, headaches were found mostly among laborers whose professional category accounted for 67.3% while senior executives represented 2.7% of consultations for headaches. Like us, Michel in his study in France, found the lowest rate among senior executives and the highest among intermediate professions [24]. Adoukonou observed that senior executives and middle executives were more prone to headaches compared to laborers [1]. This difference with Adoukonou would be partly related to the profile of his targeted companies that clearly shows that this high professional category is the most represented.
3. The clinical aspects
The majority of patients in our study (69.1%) had headaches with a precise topography. This located and fixed character of headaches as also observed by Dravé [12]. However contrary to Dravé, no patients with headaches in our study had benefited of an additional balance sheets which could help to confirm or not, like Dravé, that this fixed location is due to a secondary cause of headaches.
The evolution of headaches was chronic paroxysmal for ninety-two (92) patients and of recent appearance for the other eighteen patients (18). According to the literature [5], would be considered a priori as primary, headaches evolving on chronic mode and secondary, the headaches of recent appearance said inaugural. In our study, the clinical examination of patients had found either the presence of a general disease or a notion of a head injury, synchronous with the first headaches of eighteen (18) patients.
Regarding the timing of onset of headaches, more than two thirds (2/3) of patients complained of daytime headaches. Thereby, we can imagine the handicap that could cause the onset of headaches during work hours.
We investigated whether there were physical factors, psychological or others, which could trigger headaches. We observed that 15.5% of patients involved a particular trigger in the onset of their headaches, which factor was either physical or psychological. Dravé, also confirms the role of triggers in the onset of headaches. He observed in his study that about 41.5% of patients, with headaches investigated with CT-scan of brain, had their headaches after physical effort and/or intellectual [12]. According to Henry, Brochet and Daubech, psychological factors play an important role in the genesis and evolution of headaches, especially in chronic headaches [15].
In our study like in the study of Dravé [12], the arterial high blood pressure was the most personal history (10.9%). Young, in the newsletter of the Canadian Society of Hypertension, said: “generally severe hypertension, especially with sudden onset, would cause headaches”. However according to him, he would not also be certain that the arterial high blood pressure of grades 1 or 2 is cause of headaches. Similarly, the relationships between hypertension and primary headaches are not yet clear [39].
Finally, with the personal history and the physical examination, we distinguished probable primary and secondary headaches; 16.4% of patients had secondary headaches and 83.6 % had primary headaches. Thus, we can imagine how these primary headaches with their chronic evolution would be a daily handicap for the worker. The individualization of primary headaches distinguished the probable tension headaches for 70.7% of patients and probable migraine for others (29.3%). Brudon and Mick claim that tension headaches are among all the headaches, the most common in the general population [5]. They add that the loss of quality of life and socio-economic cost, the corollaries of this type of headaches in its chronic form should attract the attention of scientists, practitioners and the government on this condition.
4. Assessment of the quality of life (QoL) of patients with headaches
According to World Health Organization (WHO), headaches would represent a real burden on those who suffer: personal suffering, impaired quality of life and financial cost. The repeated headaches and often the constant fear of the next, would undermine family life, social life and working life [25]. WHO defines quality of life as the perception of a person of himself within the cultural environment and the value system in which he lives and according to his aspiration, difficulties and objectives that he has established [30]. The concept of QoL is enough used in the day life to such a point that intuitively every one conceives a definition, ability to take advantage of leisure activities, of enjoyments of a family life, of satisfactions obtained in the work… We also conceive that every diseases affect the QoL regarding health-related QoL. It is easy to imagine for some invalidating chronic diseases, how the physical disability which is due to them, can itself decrease the QoL. It is much more difficult, however, to measure how non-physical consequences of a disease can affect the quality of life.
Several French studies being interested in the quality of life of the migrainous patients and using various scales of evaluation of the QoL which are GRIM study in 1990 [16], Mig-Access study in 1996 [23], Hemicrania study in 1997 [22], have all concluded that the quality of life of the migrainous patients was impaired and this significantly during and outside the crisis.
In our study, to assess the QoL of patients with headaches, we used the MIDAS scale and the HIT-6 questionnaire, which estimated the degree of disability due to headaches and their impacts on the daily life of patients in their workplace. The MIDAS and HIT-6 tests have been validated as a quality of life scale of patients with headaches by several studies [20, 21, 34, 38].
D’Amico and Bussone in a clinical study using the MIDAS scale for assessing disability associated with migraine [8], found a reduction of professional performance due to headaches of 6.6 days. The average duration of work performance decrease due to headaches determined with the MIDAS scale in our study, 3.8 days – the longest disability compared to other items – shows that, like the study of D’Amico and Bussone, patients with headaches would be effectively limited in their professional activities because of their headaches.
In the study of D’Amico and Bussone [8], the distribution of patients with headaches according to four degree of increasing gravity correlated with functional disability was the most important for the 3rd degree (moderate) and 4th (severe) respectively 26.1 % and 47 %. In our study, the distribution of patients with headaches according to these four degrees of increasing gravity showed that the first (little) and second (middle) degree were the highest, respectively 42.7 % and 26.4%.
By correlating the socio-professional category with the functional disability related to headaches, we observed that the functional disability was much higher in the category of laborers than of senior executives whose functional disability was essentially little. The ergonomic benefits in workplace as well as monetary from which benefits this last category could explain this difference.
Belo and collaborators in a survey using the HIT-6 questionnaire to assess the impact on the daily lives of children with headaches in schools in Lomé, Togo [2], observed that qualitatively headaches had a negative impact on the daily lives of pupils. Jelinski and collaborators, in a study on the treatment of the migrainous Canadian patients in specialized consultation, observed that for the majority, headaches had a major impact on their daily lives [17]. In our study, near half of the patients with headaches (49.1%) had a score HIT-6 III or IV corresponding to a substantial and severe impact of headaches on their daily activities. Headaches therefore have a significant impact on activities of daily living of patients with headaches, thus impairing their quality of life.
Just like for the functional disability related to headaches, the laborers represented the socio-professional category for which headaches had the most significant impact; Similarly, senior executives are spared again about the impact of headaches on daily life.
In our study, women represent the group of patients with headaches whose the impact on daily life is more important, 42.1% against 29.7% for men. Women are also the ones whose degree of disability-related headaches was the most severe. It emerges easily that the women with headaches in the workplace are those whose quality of life is more impaired because of headaches.
CONCLUSION
Headaches impose a heavy burden to patients in the workplace, especially for women and laborers. The ergonomics in workplace and a good management of pains will improve the quality of life of patients with headaches and reduce their time of disability.
The study we conducted on headaches in the workplace is preliminary. The results of this work open the perspective for further studies, especially longitudinal, which will take into account the evolutionary aspect of headaches with treatments. This would allow to envisage solutions for an adequate management and a reduction of handicaps corollaries to this symptom for improving the quality of life and a better professional performance of patients with headaches in the workplace.
TABLES AND FIGURES
Table I: Number and distribution of workers in the different companies
| Companies |
Total number of workers |
Male |
Female |
| FASOPLAST |
170 |
156 (92%) |
14 (08%) |
| FASO COTTON |
125 |
109 (87%) |
16 (13%) |
| SODIBO/BRAKINA Ouagadougou |
342 |
317 (93%) |
25 (07%) |
| HAGE Industries |
396 |
389 (98%) |
07 (02%) |
| LONAB Ouagadougou |
225 |
146 (65%) |
79 (35%) |
| BICIAB Ouagadougou |
219 |
121 (55%) |
98 (45%) |
| TOTAL |
1477 |
1238 (83.8%) |
239 (16.2%) |
Table II: Prevalence of headaches in consultation from April to June 2011 according to the company
| Companies |
Total Consultation Number (n) |
|
Consultation for headaches |
|
|
Number(n) |
Fréquency(%) |
| FASOPLAST |
179 |
31 |
17 |
| FASO COTTON |
142 |
09 |
6 |
| SODIBO/BRAKINA Ouagadougou |
257 |
15 |
6 |
| HAGE Industries |
479 |
33 |
7 |
| LONAB Ouagadougou |
126 |
09 |
7 |
| BICIAB Ouagadougou |
212 |
13 |
6 |
| TOTAL |
1395 |
11O |
8 |
Table III: Prevalence of headaches according to the distribution of the total of each company by gender
| Companies |
Males |
Females |
| FASOPLAST |
29 (19%) |
02 (14%) |
| FASO COTTON |
05 (05%) |
04 (25%) |
| BRAKINA-SODIBO Ouagadougou |
13 (04%) |
02 (08%) |
| HAGE Industries |
32 (08%) |
01 (14%) |
| LONAB Ouagadougou |
06 (04%) |
03 (04%) |
| BICIAB Ouagadougou |
06 (05%) |
07 (07%) |
| TOTAL |
91 (07%) |
19 (08%) |
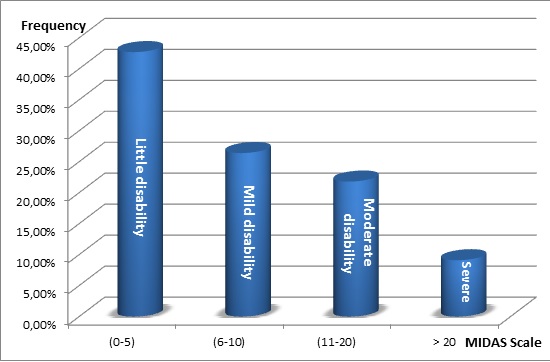
Figure 1: Distribution of patients with headaches according to the four grades of increasing severity of functional disability
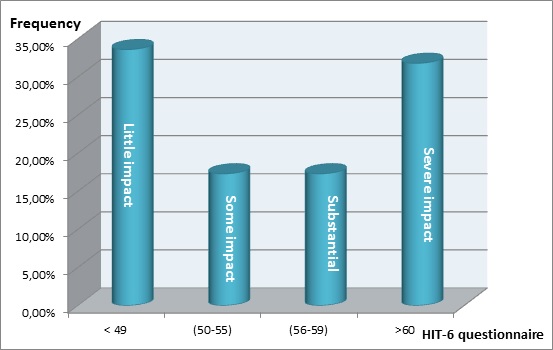
Figure 2: distribution of patients with headaches according to the impact of headaches on their activities of daily life
REFERENCES
- ADOUKONOU T A, HOUINATO D S, ADJIEN K C, GNONLONFOUN D, AVODE D G, PREUX P-M. Prévalence de la migraine dans une population de travailleurs à Cotonou au bénin. Af J Neuro Sc 2009;28(1):16-23.
- BELO M ET AL. Céphalées et qualité de vie en milieu scolaire à Lomé,Togo. Af J Neuro Sc 2009;28(2):29-34.
- BOURRIER P, PERROUX D, LANNEHOA Y, THOMAS O. Epidémiologie des céphalées de l’adulte dans les services d’urgence. In Bourrier P. Céphalées en Urgence. Collection Monographies de la Société francophone de médecine d’urgence ; Masson 2001, 234p.
- BRESLAU N, DAVIS G C, ANDRESKI P. Migraine, psychiatric disorders, and suicide attempts : an epidemiologic study of young adults. Psychiatry Res 1991; 37:11-23.
- BRUDON F, MICK G et al. Les céphalées en pratique quotidienne. John Libbey Eurotext, Paris, 2009 ; 125p.
- CELENTANO D, STEWART W F, LIPTON R B, REED M L. Medication use and disability among migraineurs : a national probability sample study. Headache 1992;32:223-8.
- D’ALESSANDRO G, POCHINTESTA N, ASSALE R, CHASTRES S G, D’ALLESANDRO R. Prevalence of migraine in the Municipality of Aosta, Italy. In: 7th International Headache seminar 2011. Neurol Sci 201;32 Suppl 1: 201-5.
- D’AMICO D, BUSSONE G. Disability and migraine : recent outcomes using an Italian version of MIDAS. J Headache Pain 2003;4:42-6.
- DONNET A, MARTINEZ S. Céphalées aux urgences : prise en charge des céphalées par le centre 15. COPACAMU 2008.
- DOUSSET V, HENRY P, MICHEL P. Epidémiologie des céphalées. Rev neurol, Paris, 2000;156(4):24-9.
- DOUSSET V, HENRY P. Céphalées chroniques quotidiennes, céphalées par abus médicamenteux, définitions, épidémiologie. Doul et Analg 2005;4:135-8.
- DRAVE A. Aspects Epidémiologiques, cliniques et tomodensitométriques des céphalées au Centre Hospitalier Universitaire Yalgado Ouédraogo (CHUYO) à Ouagadougou au Burkina Faso. Thèse de médecine, Faculté des sciences de la santé, Université de Ouagadougou, 2006, n° 042, 83p.
- EL HASNAOUI A, GAUDIN A-F. La migraine en France 10 ans après. Paris : John Libbey Eurotext ; 2004.
- GLADSTONE J, BIGAL M E. Headaches Attributable to Infectious Diseases. Curr Pain Headache Rep 2010;14:299-308.
- HENRY P, BROCHET B, DAUBECH J F. Aspects psychologiques des migraines et céphalées. Doul et Analg 1997;1, 21-6.
- HENRY P, DURU G, CHAZOT G, DARTIGUES J F et le GRIM. La migraine en France. Etude épidémiologique, impact socio-économique et qualité de vie. John Libbey Eurotext, Paris, 1993, 138p.
- JELINSKI S E, BECKER W J, CHRISTIE S N, GIAMMARCO R, MACKIE G F, GAWEL M J, ELOFF A G, MAGNUSSON J E. Clinical features and pharmacological treatment of migraine patients referred to headache specialists in Canada. Cephalalgia 2006;26:578-88.
- JENSEN R, STOVNER L J. Epidemiology and comorbidity of headache. Lancet Neurol 2008;7:354-61.
- LAVIGNE G, BLANCHET P, KHOURY S, CARRA M C, ROULEAU G, DENIS R. Céphalées et sommeil : un survol diagnostique et un guide pour le clinicien. Douleur Analg 2010 ;23:175-80.
- LIPTON RB, STEWART WF, DIAMOND S, DIAMOND ML, REED M. Prevalence and burden of migraine in the United States: data from the American Migraine Study II. Headache 2001;41:646-57.
- LUCAS C, LANTERI-MINET M, CHAFFAUT C. Comportements thérapeutiques des migraineux. FRAMIG 2000-II. Douleurs 2001;2:240-6.
- MICHEL P, DARTIGUÈS J F, LINDOULSI A, HENRY P. Loss of productivity and quality of life in migraine sufferers among French workers : results from the GAZEL cohort. Headache 1997;37:71-8.
- MICHEL P, PARIENTE P, DURU G, DREYFUS J P, CHABRIAT H, HENRY P. Mig-Access : a population-based, nationwide, comparative survey of access to care in migraine in France. Cephalalgia 1996;16:50-5.
- MICHEL P. Etude nosographique, épidémiologique et économique de la migraine en France. Thèse de Doctorat en Médecine. Bordeaux, 1991 ; N°3053.
- ORGANISATION MONDIALE DE LA SANTE (OMS). Céphalées. Aide mémoire N°277, Mars 2004.
- PARI E, RAO R, VENTURELLI E, GIPPONI S, LIBERINI P, RINALDI F, SAPIA E, PADOVANI A. Management of headache disorders in the Emergency Department setting. In: 7th International Headache seminar 2011. Neurol Sci 2011; 32 (Suppl 1): 201-5.
- POP P H M, GIERVELD C M, KARIS H A M, TIEDINK H G M. Epidemiological aspects of headache in a workplace setting and the impact on the economics loss. Eur J Neurol 2002;9:171-4.
- PREVALENCE DES CEPHALEES à travers l’enquête décennale Santé 2002-2003, France. Etudes et résultats, N°542 décembre 2006, p3.
- ROLAND M, JAMOULLE M. La céphalée en médecine générale : situation et démarche clinique. Rev Méd Brux 1996;17:288-92.
- SARACENO B. Des principes pour promouvoir la qualité de vie. My World of Multiple Sclerosis online community. 2008 Juin [Consulté le 22/06/2011]. Consultable à l’URL : http://www.msif.org/fr/publications/des_principes_pour_promouvoir_la_qualit_de_vie/preface.html
- SILBERSTEIN S-D. Advances in understanding the physiopathology of headache. Neurology 1992;42(2):6-10.
- SOMMER-BÜHLER J, DOZIER C, STALDER H. Les céphalées. Primary care 2004;4(12):244-9.
- STANG P E, OSTERHAUS J T. Migraine in the United States: data from the National Health Interview Survey. Headache 1993;33:29-35.
- Stewart WF, Lipton RB, Kolodner K, Liberman J, Sawyer J. Reliability of the migraine disability assessment score in a population-based sample of headache sufferers. Cephalalgia 1999 ; 19 : 107-14.
- Stovner L J, Zwart J A, Hagen K, Terwindt G M, Pascual J. Epidemiology of headache in Europe. Eur J Neurol 2006; 13 : 333-45.
- The international classification of headache disorders (second edition). Cephalalgia 2004 ; 24 (1) : 24-150.
- William P-P. Evaluating migraine disability : The headache Impact Test Instrument in context. Can. J. Neurol. Sci. 2002 ; 29 (2) : S11- S15.
- Yang M, Rendas-Baum R, Varon S F, Kosinski M. Validation of the headache impact test (HIT-6TM) across episodic and chronic migraine. Cephalalgia 2011 ; 31(3) : 357-67.
- Young A. Quelle est la relation entre l’Hypertension, la céphalée et la migraine ? Société Canadienne d’Hypertension Artérielle, Juin 2006 ; bulletin N°87.


