NEUROEPIDEMIOLOGY / NEUROEPIDEMIOLOGIE
SELECTIVE ATTENTION OF STUDENTS SUFFERING FROM PRIMARY HEADACHES IN A PAIN FREE PERIOD: A CASE CONTROL STUDY
L'ATTENTION SELECTIVE EN PERIODE NON DOULOUREUSE DES ETUDIANTS SOUFFRANT DE CEPHALEES PRIMAIRES : UNE ETUDE CAS-TEMOINS
- Department of Neurology, FANN Teaching Hospital, Dakar, Senegal
- Department of Neurology, Erasme Teaching Hospital, Brussels, Belgium
E-Mail Contact - FOGANG Fogoum Yannick :
ABSTRACT
Background
Headache patients frequently complain about difficulties in attention and concentration, even when they are headache-free and psychometric studies concerning attentional deficits in headache patients between attacks are scarce.
Objective
To evaluate selective attention of headache patients in a pain free period and compare them with healthy volunteers.
Subjects and Methods
We performed, between February 2011 and July 2011, a case-control study, including 45 university students consulting for primary headaches, matched with 45 healthy students as controls. Headaches were classified according to the International Headache Society criteria (IHS, 2004). Subjects with a history of brain injury, epilepsy and visual disturbancies were excluded. Mood disorders were assessed using the Hospital Anxiety Depression (HAD) questionnaire. Selective attention was evaluated using the D-KEFS color-word interference test.
Results
Mean age of patients was 23.29 ± 2.55 years, versus 22.89 ± 2.04 years for controls (p = 0.2). Migraine and tension-type headaches were the only diagnosed headache types, respectively 55.56% and 44.44%. The selective attention score was -4.04 ± 7.08 for patients, versus -1.31 ± 7.73 for controls (p = 0.02). The mean mental flexibility score was lower in headache sufferers compared to controls (36.67 ± 6.79 versus 41.33 ± 6.23, p = 0.001). Gender, anxiety and depression scores, and temporal features of headache had no correlation with selective attention score.
Conclusion
Selective attention and mental flexibility capacities seem to be reduced in primary headache sufferers in pain free period. These findings could contribute to our understanding of the pathophysiology of primary headaches.
Keywords: Selective attention, mental flexibility, neuropsychology, headache, migraine.
RESUME
Introduction
Les plaintes attentionnelles sont fréquentes chez les patients céphalalgiques, même en dehors des épisodes douloureux. Les études psychométriques sur ce sujet restent rares.
Objectifs
Notre objectif était d’évaluer l’attention sélective des patients céphalalgiques en période non douloureuse et d’identifier les facteurs l’influençant.
Patients et méthodes
Nous avons mené de Février 2011 à Juillet 2011 une étude cas-témoins incluant 45 étudiants céphalalgiques appariés selon l’âge et le genre à 45 étudiants sains. Etaient exclus tous les participants ayant des antécédents d’affection cérébrale organique ou une anomalie visuelle. Le questionnaire Hospital Anxiety Depression permettait d’évaluer le statut affectif des participants. Les céphalées étaient définies suivant les critères de l’International Headache Society (2004). Le D-KEFS Color-Word Interference Test, était utilisé pour calculer les scores d’interférence (SI 1 et SI 2) qui mesurent l’attention sélective.
Résultats
L’âge moyen des patients était de 23,29 ± 2,55 ans contre 22,89 ± 2,04 ans pour les témoins (p = 0,2). La migraine et la céphalée de tension étaient les deux types de céphalées (55,56% et 44,44% respectivement). Les symptômes d’anxiété et de dépression étaient plus fréquents chez les patients (p = 0,008 et p = 0,01 respectivement). Le score moyen de flexibilité mentale était significativement réduit chez les patients (36,67 ± 6,79 contre 41,33 ± 6,23 pour les témoins [p = 0,001]). Le SI 1 était de 3,16 ± 6,12 pour les patients contre 3,64 ± 7,47 pour les témoins (p = 0,73). Le SI 2 était de -4,04 ± 7,08 pour les patients contre -1,31 ± 7,73 pour les témoins (p = 0,02).
Conclusion
Les capacités d’attention sélective et de flexibilité mentale semblent réduites chez les patients souffrant de céphalées primaires en période non douloureuse. Ces résultats pourraient avoir des implications physiopathologiques et cliniques.
Mots-clés: attention sélective, flexibilité mentale, neuropsychologie, migraine, céphalée de tension
INTRODUCTION
Selective attention is defined as the preferential allocation of cognitive and neural resources to a specific event that has become behaviorally relevant (18). Attention is a prerequisite to all cognitive tasks and learning. It involves many brain structures grouped into the so-called attentional matrix.
Recurrent headaches are frequent and occurs in as high as a quarter of western countries population (16). In Africa, the prevalence of migraine is 3.3% in Benin (9) and 4.3% in Tanzania (26). Pain highly consumes attentional resources (14), and in chronic or recurrent forms can be associated with cognitive disorders especially in attention and memory domains (8,13). Since the last decade, rapid progress in cognitive neurosciences and functional neuro-imaging resulted in increased interest in cognitive dysfunction in pain states.
Cognitive and attentional complaints are frequent in pain free periods in recurrent pain patients (15). In recurrent headache patients, if attentional impairment is well accepted during the headache episode, reports in the literature concerning cognitive dysfunction in pain free periods are still equivocal (1,10,20,22). Patients with recurrent headaches report more depressive symptoms, but it is not clear whether psychological factors may interfere with cognitive function (12). If an attentional deficit really exists between headache episodes, it might contribute to a decreased quality of life and even socio-professional performance. For instance, in a longitudinal study from New Zealand, subjects were followed with psychometric tests from the age of 3 till the age of 26 years. Subjects diagnosed to suffer from migraine at age 26 were subtly but significantly impaired in tests of verbal ability and had a lower academic achievements (25).
Thus, the aim of the present study was to determine whether pain-free recurrent headache patients show impaired selective attentional performances compared to controls, and to identify contributing factors.
SUBJECTS AND METHODS
Subjects
This was a case-control study carried out between February 2011 and July 2011 at the Dakar University Medical Center (COUD). We included 45 students suffering from primary headaches, who consulted for headache at COUD since January 2011. They were randomly selected from the COUD data base, contacted by phone and asked to consult again in a pain free period. Controls were 45 gender- and age-matched healthy students, consulting for systematic medical screening at COUD. Headaches were classified according to The international classification of headache disorders-II (IHS, 2004) criteria (23). Participants with history of head injury, epilepsy, visual disturbances, and those receiving preventive headache medications or psychotropic drugs were excluded as well as controls with a history of recurrent headache disorder.
Ethical clearance was obtained from the Cheikh Anta Diop University Ethical Committee. A verbal consent was obtained from all participants before enrollment in the study.
Methods
Instruments
Different tools were used during the study.
Delis-Kaplan Executive Functions System (D-KEFS) word-color interference test
Selective attention is measured in tasks that involve the control of competing responses. The Stroop task provides a clear illustration of the basic capacity to focus on relevant cues concomitantly and the ability to ignore irrelevant (even conflicting) material. Given that our study sample was composed of subjects with a high level of formal education, we used a modified and more sensitive version of the Stroop task, with an additional subtask known as D-KEFS color-word interference test. This version is composed of four subtasks of increasing difficulty, each consisting of 50 items presented in random order on a sheet of paper in 5 lines of 10 items. The four subtasks are as follows:
Subtask I or Reading: 50 colour names (red, green and blue) printed in black that have to be read.
Subtask II or Naming: 50 coloured spots equally distributed among three colours (red, green and blue) have to be named.
Subtask III or Conflicting: the subject has to name the colour of the ink used to print 50 coloured names equally distributed among the three following colours: red, green and blue. The colour word rarely matches the colour of the ink used to write the colour word.
Subtask IV or Switching: the rule is identical to Subtask III except that when the colour name is surrounded with a rectangle, the colour name has to be read instead of naming the colour of the ink.
Headache questionnaire. This questionnaire was used for patients and included headache characteristics (headache periodicity, location, type, intensity, triggering factors, aggravating factors and associated symptoms) as well as past medical history, notion of treatment used, general and neurological examination.
Hospital Anxiety and Depression (HAD) questionnaire. We used a French version of the HAD questionnaire to assess anxiety and depression symptoms in subjects. HAD includes seven items for each of anxiety and depression. It is a validated tool for the assessment of mood disorders in clinical and research settings (27).
Protocol and measures. Participants were asked to consult between 09.00-11.00 am after a normal night sleep. Data were collected with calm and relaxed subjects in a quiet room, well illuminated, with temperature around 25°C. Socio-demographic data were obtained for all subjects. Patients were asked questions on the characteristics of their headaches. They then underwent a general and neurological examination. Headaches types were classified according to these data. The HAD questionnaire was filled in by all subjects, and the anxiety and depression scores were obtained for every subject.
The D-KEFS color-word interference test was then administered. All subjects were informed that they were going to perform an attentional test and no details about our assumptions were provided before the test. At each subtask, the subjects were asked to name as quickly and accurately as possible. Each subtask was preceded by a practice trial of 10 stimuli in order to familiarize the subject with the procedure and in order to ensure that instructions had been well understood. The duration to perform each subtask was 45 seconds, measured with a chronometer. Outcome measures from the attentional task were number of words named and number of errors (incorrect colour naming or reading) for each of the four subtasks.
Two additional outcome measures were interference scores 1 and 2. Interference score is designed to reveal the increase in time for reacting to colours caused by the presence of conflicting colour word stimuli and is thus a measure of the interference of colour words upon naming colour (20). Interference scores are measures of selective attention, and were obtained as follows with the Golden formula (7).
IS 1 = S3 – S predict IS 2 = S4 – S predict
with S predict = (S1 × S2) : (S1 + S2)
IS indicates interference score ; Sn indicates score for subtask n
Patients were asked if they felt any head pain before, during and at the end of the tests.
Statistical analysis
Data were encoded in the CS pro 3.0 software, and analyzed using SPSS 16.0 software.
Means were compared with ANOVA. A p-value < 0.05 was used as significance threshold.
The correlation between clinical, affective and cognitive variables were analyzed using the Spearman test.
RESULTS
Characteristics of the study population
Socio-demographic characteristics [Table I]. We included in our study 45 cases (recurrent headache patients) and 45 healthy controls. The male : female sex-ratio was 2 : 3 in the two groups. Age of the participants ranged from 19 to 30 years. Mean age of all the participants was 23.09 ± 2.35 years. Mean age was 23.29 ± 2.55 years for the patients’ group, and 22.89 ± 2.04 years for controls (p = 0.2). All the participants were University students.
Headaches features [Table II]. Patients were diagnosed as having migraine or tension-type headache (TTH). The frequencies of migraine and tension-type headache were respectively 55.56% and 44.44%. The migraine subtypes were migraine without aura in 22 (88%) of patients and migraine with visual aura in 03 (12%) patients. Concerning TTH, the frequencies of sub-types were 55% for episodic TTH and 45% for chronic TTH. The mean number of headache days per month in patients was 12.58 ± 7.44 days. The mean delay from the end of the last headache episode to consultation was 4.29 ± 5.57 days with a range from 0.5 to 30 days.
Anxiety and depression. Anxiety and depression symptoms were more frequent in patients than controls (p = 0.0008 and p = 0.01 respectively) [Table I]. The scores of patients and controls on HAD questionnaire did not correlate with interference scores 1 and 2 (r = -0.06 ; p = 0.55 and r = -0.02 ; p = 0.8 respectively).
Comparisons
Comparison of mean scores at different sub-tasks of D-KEFS Color-Word Interference Test [Figure 1]. Patients had a mean score of 93.6 ± 14.61 at subtask 1 (reading), significantly lower than that of controls reaching 101.93 ± 21.69 (p = 0.03). At the subtask 2 (naming), the patients mean score was 72.6 ± 10.91 versus 75.51 ± 10.6 for controls (p = 0.2). On subtask 3 (conflicting) the patients mean score was 43.87 ± 8.23 versus 46.29 ± 7.03 (p = 2.14). However, on subtask 4 (switching), the patients’ score was 36.67 ± 6.79, significantly lower than 41.33 ± 6.23 for controls (p = 0.001). However, patients’ scores at subtasks 1 and 4 did not correlate with anxiety and depression scores (r = 0.11; p = 0.49 and r = -0.08; p = 0.60 respectively).
Interference scores [Figure 2]. The interference score is a measure of selective attention. The mean interference score 1 was 3.16 ± 6.12 for patients versus 3.64 ± 7.47 for controls, and there was no significant difference between the two groups (p = 0.73). The mean interference score 2, was -4.04 ± 7.08 for patients against -1.31 ± 7.73 for controls (p = 0.02). Interference scores 1 and 2 for migraine and TTH patients were not significantly different (p = 0.53 and p = 0.67 respectively). There was also no significant difference between interference scores 1 and 2 of patients with episodic or chronic headaches (p = 0.66 and p = 0.86 respectively). Examination within or after 48 hours of the end of the last headache episode was not associated with significant change in interference scores 1 and 2 (p = 0.80 and p = 0.21 respectively). Anxiety and depression scores of patients and controls did not correlate with interference scores 1 and 2 (r = -0.06; p = 0.55 and r = -0.02 ; p = 0.8 respectively).
Errors. Mean number of errors (defined as incorrect color naming or reading) increased across the four subtasks, from 0.56 ± 0.69 to 2.13 ± 1.14 in the patients’ group, and from 0.47 ± 0.78 to 1.71 ± 1.18 for controls. At subtask 1 (reading) and subtask 2 (naming) there was no significant difference in the number of errors in the two groups (p = 0.57 and p = 0.09 respectively). However at subtask 3 (conflicting) and subtask 4 (switching) that need more attentional resources, patients committed more errors than controls (p = 0.04 and p = 0.03 respectively).
DISCUSSION
Although the prevalence of headache disorders in many countries is high (17), and cognitive complaints of headache patients frequent (15), studies on cognitive functioning of headache patients are still scarce and equivocal. This study revealed that selective attention and mental flexibility of primary headache patients are impaired in a pain-free period. In other words, the abilities of these patients to focus on a specific task and to switch from one task to another are altered compared to their healthy controls in the pain-free period.
The D-KEFS word color interference test subtasks are of increasing difficulties. Mean scores of headache patients at any subtask of the D-KEFS word color interference test were inferior to those of controls, showing a reduced speed in completing different subtasks. The significantly lower performances of patients at substasks 1 (reading) can be attributed to a prolonged reaction time in the initiation of cognitive and motor processes (20). At subtask 4 (switching) which requires more attentional resources, the capacity of patients to switch from one task to another was altered compared to their healthy controls. Grisart and colleagues in a study using the same version of Stroop test, found no difference of scores in subtask 4 between chronic pain patient with mild pain intensity and controls (8). However the latter study included mainly chronic low back pain patients without headaches. Headache patients might thus be more prone to difficulties in mental flexibility. The prefrontal dorso-lateral cortex is particularly involved in tasks requiring mental flexibility. Recently, an altered functional connectivity in the left prefrontal lobe of migraineurs without aura in pain free state was found using brain imaging techniques (11).
Interference score is a measure of selective attention (21). Primary headache patients had numerically lower selective attentional scores than controls and this difference was significant only for interference score 2 which is more sensitive (21). Mulder and colleagues found reduced attentional performances in a pain free period in migraineurs with aura and not in migraineurs without aura (20). The use of a less sensitive version of stroop test by Mulder and colleagues can explain the discrepancy between our results. The small number of patients with migraine with aura included in our study did not allow us to evaluate selective attention specifically in this subgroup. Gijsen and colleagues using the Stroop test in a population including many pain categories, found that decreased selective attention score was correlated to pain intensity, except with headache where pain free patients showed significantly reduced interference score (6). This last result suggest a specific cognitive processing in recurrent headache patients compared to other pain syndromes. Villa and colleagues found reduced visuo-spatial attentional capacities in migrainous children during pain-free periods compared to controls (24). Although spatial and color selective visual attention are different, they share common neural networks in the attentional matrix (18).
Interference scores were not associated with headache type and frequency, post- or inter-ictal states. Headache characteristics seem to have no effect on interference scores (3,5,22), with the notable exception of the presence of an aura in migraine (20).
Anxiety and depression symptoms were more frequent in the group of headache patients. This is in accordance with other studies (2,6,8). Non-headache factors, and psychiatric comorbidity especially, had been correlated by some authors to cognitive performances in primary headache patients (5). However, many studies, reported no association between anxiety and depression scores on one hand, and interference scores in primary headache patients on the other hand (4,6,8,12,19).
A limitation to this study is the relatively small sample size of subjects. We believe nonetheless that our results are valid because of the matched control group and the use of a more sensitive tool to detect selective attention deficits.
From a clinical and practical point of view it is important to realize that the experience of recurrent headache may influence selective attention in the pain free period. Our understanding of the effects of recurrent headache on cognitive functioning has important implications for appreciating the range of problems reported by patients with headache, and for understanding the pathophysiology of primary headaches. However, there remains a need for a larger study, involving more patients, to confirm our findings.
ACKNOWLEDGEMENTS
We thank all the patients and health care professionals involved.
FUNDING
This research received no specific grant from any funding agency in the public, commercial, or non-profit sectors.
CONFLICT OF INTEREST
The authors declare that there is no conflict of interest.
Table I: Socio – demographic data, anxiety and depression scores of subjects groups.
| Characteristics |
Study sample |
Patients |
Controls |
P |
| N |
90 |
45 |
45 |
|
| Age range (years) |
19-30 |
19-30 |
19-28 |
|
| Sex-ratio (M : F) |
2 : 3 |
2 : 3 |
2 : 3 |
|
| Mean age (years) |
23.09 ± 2.35 |
23.29 ± 2.55 |
22.89 ± 2.04 |
0.2 |
| *HAD-A score |
9.82 ± 3.74 |
11.11 ± 3.66 |
8.53 ± 3.39 |
0.0008 |
| µHAD-D score |
6.12 ± 3.47 |
6.98 ± 3.65 |
5.27 ± 3.09 |
0.01 |
Mean ± SD
*Anxiety score to HAD (from 0 to 21)
µDepression score to HAD (from 0 to 21)
Table II: Interference score of patients according to the type, frequency and delay after the last episode of their headache.
N (%)
| Migraine Patients |
25 (55.56%) |
3.67 ± 5.73 |
-4.44 ± 7.20 |
| µ TTH patients |
20 (44.44%) |
2.51 ± 6.67 |
-3.53 ± 7.08 |
| p value |
|
p = 0.53 |
p = 0.67 |
| Chronic headache |
19 (42.22%) |
3.36 ± 7.01 |
-3.49 ± 5.86 |
| Episodic headache |
26 (57.78%) |
3.02 ± 5.52 |
-4.45 ± 7.94 |
| p value |
|
p = 0.86 |
p = 0.66 |
| *DLE ≥ 48h |
27 (60%) |
3.44 ± 5.83 |
-5.67 ± 8.28 |
| DLE< 48h |
18 (40%) |
2.97 ± 6.41 |
-2.95 ± 6.28 |
| p value |
|
p = 0.80 |
p = 0.21 |
Mean ± SD
$IS 1: Interference Score 1; $$IS 2: Interference Score 2
*DLE: Delay to the last episode of headache; µTTH: Tension-type Headache
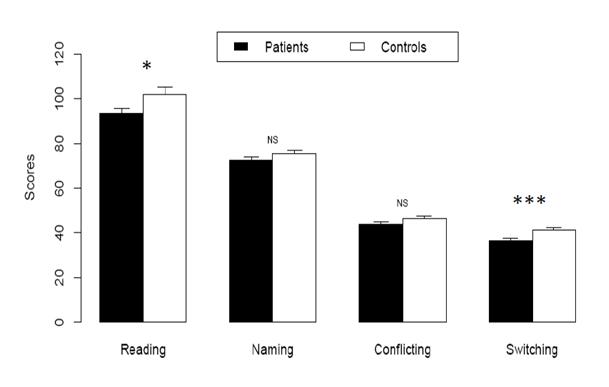
Figure 1: Mean (± 95% CI) scores of patients and controls at different sub-tasks of D-KEFS
*p = 0.02, NS: non significant difference.
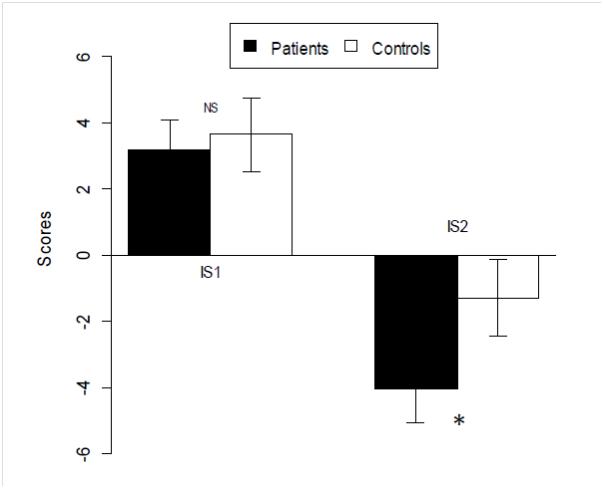
Figure 2: Mean (± 95% CI) interference scores of patients and controls at the D-KEFS Word-Color Interference test
*p = 0.03, ***p = 0.001, NS: non significant difference.
REFERENCES
- BAARS MA, VAN BOXTEL MP, JOLLES J. Migraine does not affect cognitive decline: results from the Maastricht aging study. Headache 2010;50: 176-84
- BRESLAU N, SCHULTZ LR, STEWART WF, et al. Headache and major depression. Is the association specific to migraine? Neurology 2000;54: 308-13
- CALANDRE EP, BEMBIBRE J, ARNEDO ML, et al. Cognitive disturbances and regional cerebral blood flow abnormalities in migraine patients: their relationship with the clinical manifestations of the illness. Cephalalgia 2002;22: 291-302
- ECCLESTON C. Chronic pain and distraction: An experimental investigation into the role of sustained and shifting attention in the processing of chronic persistent pain. Behavioral Research and Therapy 1995;33: 391-405
- GAIST D, PEDERSEN L, MADSEN C, et al. Long-term effects of migraine on cognitive function: a population-based study of Danish twins. Neurology 2005;64: 600-7
- GIJSEN CP, DIJKSTRA JB, VAN BOXTEL MPJ. Recurrent pain is associated with decreased selective attention in a population-based sample. PAIN 2011;152: 188-93
- GOLDEN CJ. The diagnosis of brain damage by the Stroop test. Journal of Clinical Psychology 1976;32: 654-8
- GRISART JM, PLAGHKI LH. Impaired selective attention in chronic pain patients. Eur J Pain 1999;(3): 325-33
- HOUINATO D, ADOUKONOU T, NTSIBA F, ADJIEN C, AVODE DG, PREUX PM. Prevalence of migraine in a rural community in south Benin. Cephalalgia. 2010;30(1):62-7
- JELICIC M, VAN BOXTEL MPJ, HOUX PJ et al. Does migraine headache affect cognitive function in the elderly? Report from the Maastricht aging study (MAAS) Headache 2000;40: 715-9
- JIN C, YUAN K, ZHAO L, ZHAO L, YU D, VON DENEEN KM, ZHANG M, QIN W, SUN W, TIAN J. Structural and functional abnormalities in migraine patients without aura. NMR Biomed. 2013;26(1): 58-64
- KALAYDJIAN A, ZANDI PP, SWARTZ KL et al. How migraines impact cognitive function: findings from the Baltimore ECA. Neurology 2007;68: 1417-24
- KUHAJDA CM, THORN BE, KLINGER MR et al. The effect of headache pain on attention (encoding) and memory (recognition). PAIN 2002;97: 213-21
- LEGRAIN V, VAN DAMME S, ECCLESTON C et al. A neurocognitive model of attention to pain:behavioural and neuroimaging evidence. PAIN 2009;144: 230-2
- LEIJDEKKERS MLA, PASSCHIER J, GOODSWAARD P et al. Migraine patients cognitively impaired? Headache 1990;30: 352-8
- LIPTON RB, STEWART WF, DIAMOND S et al. Prevalence and burden of migraine in the United States: data from the American Migraine Study II. Headache 2001;41: 646-57
- MATEEN FJ, DUA T, STEINER T et al. Headache disorders in developing countries: research over the past decade. Cephalalgia 2008;28 (11): 1107-14
- MESULAM M. Attentional and confusional states. Continuum Lifelong Learning Neurol. 2010;16 (4): 128-39
- MONGINI F, KELLER R, DEREGIBUS A et al. Frontal lobe dysfunction in patients with chronic migraine: a clinical-neuropsychological study. Psychiatry Res. 2005;133: 101-6
- MULDER EJ, LINSSEN WH, PASSCHIER J et al. Interictal and postictal cognitive changes in migraine. Cephalalgia 1999;19: 557-65
- STROOP. A Studies of interference in serial verbal reactions. J Exp Psychol. 1935;18:643-62
- SUHR JA, SENG EK. Neuropsychological functioning in migraine: clinical and research implications. Cephalalgia 2011;32(1):39-54
- The Headache Classification Committee of the International Headache Society. The International Classification of Headache Disorders, 2nd edn. Cephalalgia 2004;24 (Suppl. 1):1-160
- VILLA TR, CORREA MAR, DIAZ LAS et al. Visual attention in children with migraine: a controlled comparative study. Cephalalgia 2009;29: 631-4
- WALDIE KE, HAUSMANN M, MILNE BJ, POULTON R. Migraine and cognitive function: a life-course study. Neurology 2002;59(6):904-8
- WINKLER AS, DENT W, STELZHAMMER B, KERSCHBAUMSTEINER K, MEINDL M, KAAYA J, MATUJA WB, SCHMUTZHARD E. Prevalence of migraine headache in a rural area of northern Tanzania: a community-based door-to-door survey. Cephalalgia. 2010;30(5):582-92
- ZIGMOND AS, SNAITH RP. The hospital anxiety and depression scale. Acta Psychiatrica Scandinavica 1983;67:361-70