
|
|
|
CASE REPORT / CAS CLINIQUE
SELF-INFLICTED TRANSPARIETAL INTRAVENTRICULAR NAIL: CASE REPORT AND SURGICAL TECHNIQUE
AUTO-INFLICTION TRANSPARIETALE ET INTRAVENTRICULAIRE D'UN CLOU: RAPPORT DU CAS ET TECHNIQUE CHIRURGICALE
E-Mail Contact - UDOH David Okon :
daveudoh@yahoo.com
ABSTRACT Background Methods Results Conclusion Key Words: Intracranial Nail; Open Cranial Procedure; Psychiatric Evaluation RÉSUMÉ Contexte Méthodes Résultats Conclusion Mots Clés: Clou Intracrânien ; Plaie crânio- cérébrale;Technique chirurgicale ; Psychiatrie INTRODUCTION Unusual cranio-cerebral injuries with penetrating nail are more commonly inflicted with nail guns in Europe and America [1,3,2,9,13,5]. Occasional cases of hand-driven nails occur in underdeveloped countries, though very rare [10,6,14]. We present one patient with a self-inflicted intracranial nail injury emphasizing thorough pre-operative radiological, neurosurgical and psychiatric evaluation. We also describe our approach to intraoperative management and nail retrieval devoid of risks of further injury. MATERIALS AND METHODS/ CASE MATERIAL Case summary A 27-year old unemployed right-handed Nigerian male presented two days after driving a10cm long nail through his own skull using a thick block of wood held in the right hand. He complained of vertical headaches and right-sided weakness. A 3-cm rusty nail-head jutted out 2cm left of the vertex. His Glasgow coma score was 15, but he had right dysgraphaesthesia and spastic hemiparesis worse in the lower extremity. Psychiatric evaluation revealed social problems and chronic depression. He was commenced on antidepressants. Cranial computerized tomography (fig.1) showed a transparietal nail (with its distal end in the body of the left lateral ventricle) associated with pneumocephalus and cerebritis. He had a limited left parietal craniectomy with abscess evacuation and retrieval of nail. Pre-operative neurological impairments improved and he has remained well on neurosurgical and psychiatric follow-up. Details of operative treatment (fig.2) Under endotracheal anaesthesia with muscle relaxation, an extended parietal flap was raised across the midline to the right and encircling the nail. Cranial nail entry point exposed, a 4cm radius half-circle craniectomy was centred on the nail (which was still held by an intact bony spur to control its movement) – with the base of the half-circle craniectomy on the midline for access to the superior sagittal sinus. Durotomy was completed with a radial incision freeing the nail from dura. Using hand-held retractors with narrow blades, the intraparenchymal course of the nail was exposed to the body of the lateral ventricle; 10 ml of abscess was evacuated around the nail for microbiology. With the entire extra- and intracranial extent of the nail in view, the bony spur securing the nail was finally excised to retrieve the nail. Copious irrigation was done with ceftriazone-constituted warm saline irrigation fluid. Durorapphy was carried out with interrupted vicryl and scalp was apposed with interrupted nylon stitch. Antibiotics were continued for four weeks. Left hemiparesis worsened after surgery, but improved gradually to normal power with physiotherapy. His mood improved with antidepressants and he was discharged to out-patient for follow up. He has remained well after four years of follow-up at the neurosurgical and psychiatric out-patient departments. DISCUSSION Penetrating cranio-cerebral injuries, on the whole, are uncommon in civilian practice [1, 3, 10, 7, 12]. Penetrating injury to the brain is usually accidental or suicidal, self infliction being more common than accidental discharges [1, 5]. Some intracranial nails have been successfully removed with skull radiographs as the sole radiological evaluation, and without CT [14]. The latter is, however, important to demonstrate the extent and direction of the nail, involved neurovascular structures and associated parenchymal lesions (haemorrhage, abscess or aneurysm); it is important as well for operative planning and the prediction of postoperative neurological sequelae [2,8,4]. A combination of CT and angiography as preoperative examination will give assurance of safety in these cases, showing aneurysms, extravasations, etc[9, 5, 11]. The primary pre-operative concern is the formation of a traumatic pseudoaneurysm; this prompts both preoperative and follow-up cerebral angiography- for haematomas and aneurysms may not be seen on initial scans[9,11]. Although most patients presenting to the hospital with intracranial nail survive with good mental status, those with major vascular damage, brain stem or diencephalic injury may not. The route of entry, thus, is important: Nail injuries through the roof of the mouth into the skull base could be fatal [8]. For those patients who survive, clinical decision making should focus on preventing further cortical or vascular damage and rational management strategy should permit discharge without further injury [13, 5]. There are reports of intracranial nails removed under sedation or local anaesthesia, with gentle rotatory movements or through a burr hole[10, 14]. However, an open cranial procedure permits exposure of the whole nail length, elevation of depressed skull fracture, abscess evacuation and visualization of vascular structures and aneurysms [5]. CONCLUSION Self-inflicted hand-driven intracranial nail is a very rare form of penetrating cranio-cerebral trauma preoperative computerised tomography scan of the brain; meticulous open cranial removal and psychiatric management enable discharge without further injury or deficits. 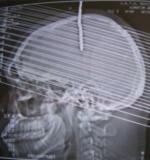 Figure 1: cranial computerized tomography scans brain (sagittal)  Figure 2: Cranial computerized tomography scan brain (coronal) 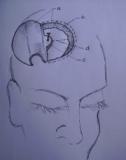 Figure3: Illustration of operative technique a: scalp flap (extended 3cm across the midline to the right) and edge of scalp incision b:outer (left parietal) edge of craniectomy c:bone spur (at the right parietal edge of craniectomy opening) left to support the nail prevent its movement during exposure of the intracranial course of the nail d:dura mater and dural incisions REFERENCES
|
© 2002-2018 African Journal of Neurological Sciences.
All rights reserved. Terms of use.
Tous droits réservés. Termes d'Utilisation.
ISSN: 1992-2647