CASE REPORT / CAS CLINIQUE
ACUTE APPENDICITIS FOLLOWING VETRICULOPERITONEAL SHUNT SURGERY FOR HYDROCEPHALUS DUE TO AN INTRACRANIAL SPACE OCCUPYING LESION
- Division of Neurosurgery, Department of Surgery, Kenyatta National Hospital, University of Nairobi, Nairobi, Kenya
E-Mail Contact - MWANG’OMBE N. J. M. :
SUMMARY
Ventrieulo-periloneal shunt placement is a common operation in the Neurosurgical unit at the Kenyatta National Hospital, Nairobi. The common complications of shunt surgery are infection and obstruction. A case of acute appendicitis following vcntriculoperitoneal shunt placement in a patient with hydrocephalus secondary to an intracranial tumour treated at the Kenyatta National Hospital is presented. Although other intra-abdominal complications such as gut perforation, peritonitis and trans-recta] migration of the peritoneal shunt tip are commonly seen in the unit, acute appendicitis in a patient with ventriculoperitoneal shunt has not been previously reported. While this association may have been incidental it is also possible that the presence of the peritoneal shunt precipitated the attack of acute appendicitis.
Kewywords : Hydrocephalus, VP Shunt, Acute Appendicitis
RESUME
Les derivations ventriculo-peritoneales sont couramment effectuees dans Ie service de Neurochirurgie de l’hopital National Kenyatta a Nairobi. Les complications habituelles d’une telle chirurgie, sont d’ordre infectieux et concernent l’obstruction de la valve. Un cas d’appendicite aigue consecutif a la mise en place d’une telle valve chez un patient ayant une hydrocephalie secondaire a une tumeur intracranienne traitée dans cet hopital est rapporte ici. Les complications abdominales hahiluellement observees sont des perforations aigues, des peritonites ou des migrations transrectales du materiel de prothese mis en place; une appendicite aigue n’a jamais ete constatee. Il est possible qu’il s’agisse simplement d’une association mais il est possible aussi que la presence d’un tel materiel peritoneal ait favorise la survenue d’une appendicile aigue.
INTRODUCTION
Hydrocephalus is a condition of multiple aetiology in which cerebrospinal fluid (csf) produced in the ventricles of the brain is not absorbed in a normal fashion. This causes enlargement of ventricular system which generally results in intra-cranial hypertension or increase in head size in children. In the paediatric age group, the diagnosis is based on measurement of head circumference, ultra-sound and computed tomography scanning which shows ventriculomegally. Management is placement of shunt diversion system (generally from the ventricles to the abdominal cavity). Die common complications are infection and obstruction requiring reoperation (1).
Acute appendicitis was described by Reginald Fitz in 1886 and he introduced the term « appendicitis ». He recommended that acute appendicitis should be treated by a surgeon before the appendix reptured. (2)
This surgical approach is still standard today. Appendicitis is an inflammation of the appendix and a common cause of acute abdomen. It occurs at any age but is commonest in the younger age group. The classic history is the onset of central abdominal pain. Often associated with vomiting which localizes to the right iliac fossa. Examination may show a distressed patient who is febrile, has a coated tongue with foetor oris and has abdominal tenderness to palpation which is maximal in the right iliac fossa. This is usually associated with guarding and rebound tenderness may be present. A full blood count may show a raised white cell count with a neutrophilia. (3).
A 24 year old African male developed acute appendicitis one month following VP shunt placement. The shunt was placed to treat hydrocephalus caused by a brain tumour. One month after placement of the VP shunt he was readmitted with an acute abdomen. Clinical diagnosis of acute appendicitis was made, emergency surgery performed and an inflamed appendix removed. In this paper details of this case are presented and an attempt is made to explain this unusual association.
CASE REPORT
A 24 year old African male was admitted to the Neurosurgical unit at Kenyatta National Hospital. Nairobi, Kenya, with a foLir month history of headache, vomiting and blurred vision. Fundoscopy revealed bilateral papilloedcma. His level of consciousness was normal and his memory was not impaired. A part from a slurred speech he had no other neurological defits. A CT scan of the head confirmed a tumour in the pineal region with associated hydrocephalus (figl).
He underwent ventriculoperitoneal shunt placement with improvement of symptoms. One month after he was discharged from hospital to await external beam radiation to the tumour, he was readmitted to the unit with a three day history of severe abdominal pain and diarrhea. He had a temperature of 37.5 degrees C, BP I 10/80 and a heart rate of 96/min. He had a tenderness and guarding at Me Bourney’s point and rebound tenderness was elicited. Bowel sounds were present. He had an HB of 1 3.4g/dl, WBC 15.1xl9/L,Na 139, K4.7, cl 105 and Urea 4.2. A diagnosis of acute appendicitis was made. He was taken to theatre and under a general anaesthetic a gridiron incision through Mc Burney’s point in the right iliac fossa was made and an inflamed appendix removed. There was pus in the para-caecal area. Cultural of the pus did not grow any organisms. The tip of the shunt was found to lie near the para-caecal area and was draining clear csf. Culture of a sample of the csf was negative. He was put on broad spectrum antibiotics post-operatively. Histological examination revealed an inflamed appendix. He made a good recovery and was discharged from hospital seven days later.
DISCUSSION
VP shunt placement has the highest incidence of complications of all neurosurgical procedures. Common complications ofVP shunting are obstruction, infection, exit from peritoneal cavity and perforation of viscus.
(I). Shunt procedures may be necessary in a patient with an inoperable pinealoma who has ventriculomegally (4). Acute appendicitis is a common cause of an acute abdomen, ll can occur at any age but is commonest in the younger age group. The classic history is the onset of central abdominal pain, often associated with vomiting, which localizes to the right iliac fossa. Common differential diagnosis include pelvic inflammatory disease, mesenteric lymphadenitis, gastroenteritis, Yersinia enterocolitis, urinary tract infection, renal colic, ectopic pregnancy, panacrcatitis, divcrticulitis, mittelschmerz, perforated duodenal ulcer and cholecystitis. Rarer differential diagnosis include Meckel’s diverticulitis, torsion of ovarian cyst and small bowel obstruction. Acute appendicitis following VP shunt surgery is unusual. Other infra abdominal complications such as ascites, intestinal perforation with peritonitis and pscudocyst formation have been reported after VP shunting (1). A disturbance in the blood brain barrier (BBB) seen in patients with intracranial tumours may lead to elevation of csf protein and failure of peritoneal absorption of csf after shunt placement and ascites. Peritoneal metastases may also play a role in the development of ascites associated with medulloblastomas and pineoblastomas. (5). The incidence of shunt infections ranges from 2-27%.
The clinical illness may vary from a low-grade fever to fulminant ventriculitis and sepsis. Comnon organisms are coagulase-negative staphylococci (staph epidermidis) which account for more than half of shunt infections, staph aureus (the second most common organism), gram negative (enteric) bacilli, enterecocci and propionibacterium acnes. (6). Systemic antibiotic therapy alone may be effective in low grade shunt infection. In fulminant shunt infection surgical removal of the shunt is necessary. (7).
The lumen of the appendix may be blocked by a piece of stool, swallowed foreign body or intramural swelling from an infection, resulting in swelling of the whole appendix which becomes prone to infection by bacteria. If the infected appendix is not removed an abscess may form and eventually burst or perforate. Anaerobes which are normal flora of the large bowel, are commonly associated with acute appendicitis. Facilitating pathologic process which may lead to anaerobic infections are compromised vascular system, trauma, tissue destruction and antecedent infections resulting in necrosis. (3). The common pathogen are Bacteroides, Fusobacterium, Anaerobic cocci and Peptostreptococcus.
The association between VP shunt placement and acute appendicitis in this patient may have been incidental, However, a low grade shunt infection may cause infection and swelling of the appendix and lead to acute appendicitis. A shunt tube within the peritoneal cavity pressing on the appendix may compromise the vascular system of the appendix and lead to anerobic infection within the appendix and appendicitis. Both these factors may probably have played a role in the development acute appendicitis in this patient.
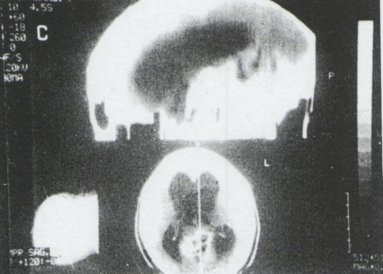
Figure 1
REFERENCES
- RAIMONDI, A.J., ROBINSON, J.S., KUWAMURA, K. Complications of ventriculoperitoneal shunts and a critical comparison of the three piece and one piece systems. Child’s Brian 3:321-342, 1977.
- FITZ, R.H., perforating inflammation of the vermiform Appendix with special reference to its early diagnosis and treatment. AMJ Med Sci 92: 321-346, 1886.
- TEMPLE, C.L., HUCHCROFT, S.A., TEMPLE, W.J., The natural history of appendicitis in adults. A prospec tive study. Annals of surgery. 221 (3): 278-81, 1995.
- RAIMONDI, A.J., TOMITA, T., Pineal Tumours in childhood Epidemiology, pathophysiology and Surgical approaches. Child’s Brain., 9 (3/4): 239- 266, 1982.
- ADEGBITE, A.B., KHAN, M., Role of protein content in CSF ascites following ventriculoperitoneal shunting. Case report J. Neurosurgery 57: 423-425, 1982.
- JAMES, H.E., WALSH, J.W., WILSON. H.D., Connor, J.D., BEAN, J.R., TIBBS P.A., Prospective randolmised study of therapy in cerebrospinal fluid shunt infection. Neurosurgery 7: (5) 459-463,1980.
- OBRIEN, M., PARENT, A., DAVID, B., Management of ventriculoperitoneal shunt infections. Child’s Brain 5: 304-309, 1979.