
|
|
|
CASE REPORT / CAS CLINIQUE
ANTERIOR CERVICAL OSTEOPHYTES CAUSING DYSPHAGIA : A CASE REPORT
DYSPHAGIE PAR OSTEOPHYTES CERVICAUX ANTERIEURS : UN CAS CLINIQUE
E-Mail Contact - SALEM-MEMOU Sidi :
fkct@hotmail.com
ABSTRACT Background: Large osteophytes can produce otolaryngological symptoms such as dysphagia, dysphonia, and foreign body sensation. Anterior cervical osteophyte can occur in degeneration of the cervical spine or in diffuse idiopathic skeletal hyperostosis (DISH), also known as Forestier’s disease. Case report: The patient in this case experienced a rapid resolution of dysphagia following the resection of protuberant cervical osteophytes using a standard anterior approach. There were not post operative complications. Conclusion: This clinical entity should be included among the differential diagnoses of dysphagia in elderly adult patients. Keywords: Cervical osteophytes, Dysphagia, diffuse idiopathic skeletal hyperostosis (DISH), osteophytectomy INTRODUCTION Anterior cervical osteophytes have a prevalence of 20-30% in the elderly population. (1) Causes of cervical osteophytes include diffuse idiopathic skeletal hyperostosis, ankylosing spondylitis, degenerative changes, and prior trauma, including surgery. (16) Diffuse idiopathic skeletal hyperostosis (DISH) or Forestier disease involves hyperostosis of the spinal column. The prevalence of DISH is quite variable and ranges between 2.9 and 28%. (10, 20) DISH is known as one of the most common causes of anterior cervical hyperosteophytosis induced dysphagia that requires the surgical intervention. (2) It is estimated that 3% of individuals over the age of 40 have DISH and 0.1-6% of those will develop dysphagia. (3) In this case report, we describe a surgically treated 67-year-old man with dysphagia caused by a huge anterior cervical osteophyte due to DISH. CASE REPORT A 61-year-old man had had mild dysphagia for several years. During six months before admission, the dysphagia worsened and gradually progressed to dysphagia to liquids, and he had prevalent neck pain. The patient had no history of trauma to the neck. His past medical history included type 2 diabetes mellitus and high blood pressure. He had no dysphonia or dyspnea but did have some odynophagia on swallowing. Upon examination the patient had no neurological signs in the upper or lower limbs. There were no signs of arthrotic cervical myelopathy. Routine blood tests were also normal. Noncontrast cervical computed tomography (CT) showed a large osteophyte formation, spanning from C2 to C5 anteriorly with the largest osteophyte at C2-C3 impinging on the esophagus (figure 1). The difficulty in swallowing was attributed to the compression of the esophagus by the cervical osteophytes. The surgery was performed via an anterolateral approach in the neck using the usual technique. The giant anterior osteophyte was removed with rongeurs and a high speed drill until the anterior spinal surface from C2 to C4 was flat. The lower part of the osteophyst (C4-C5) was respected, because in our opinion it was not at the origin of compression of the esophagus. His resection was not interesting. Moreover, it will further weaken the spine. No fixation was done as the disc space was kept intact and there was no instability. There were not post operative complications. A postoperative CT of the cervical spine demonstrated removal of the anterior cervical osteophyte (figure 2). The patient reported significant improvement of dysphagia immediately postoperatively and complete resolution of symptoms at his two-month follow-up. DISCUSSION Dysphagia is a swallowing disorder that manifests as difficulty passing the food bolus through the esophagus. It is a frequent cause of medical appointments. Mosher, in 1926, was the first to describe dysphagia caused by osteophytes. (12) Dysphagia secondary to cervical osteophytes is an overall rare event. However, there are documented cases of dysphagia, dysphonia, dyspnea, and obstructive sleep apnea secondary to hyperostosis of the cervical spine. (6,9,17) Anterior cervical osteophytes have a prevalence of 20-30% in the elderly population. (1) Causes of cervical osteophytes include diffuse idiopathic skeletal hyperostosis, ankylosing spondylitis, degenerative changes, and prior trauma, including surgery. (16) In our case, the most probable diagnosis was diffuse idiopathic skeletal hyperostosis (DISH or Forestier disease) because C2-C5 vertebral bodies were fused by the anterior bony spur and intervertebral disc height was relatively preserve. Forestier’s disease is a degenerative pathology of unknown cause responsible for ossification of the entheses. The radiographic diagnosis for DISH proposed by Resnick and Niwayama (also known as the Resnick criteria) is comprised of the following three criteria: the presentation of flowing calcification and ossification of the anterolateral aspect of four contiguous vertebral bodies, preservation of intervertebral disk height in the involved segments without radiographic changes of degenerative disk disease, and absence of intervertebral or apophyseal joint ankylosis and degeneration, sclerosis, or intra-articular osseous fusion. (15) DISH is known as one of the most common causes of anterior cervical hyperosteophytosis induced dysphagia that requires the surgical intervention. (2) It is estimated that 3% of individuals over the age of 40 have DISH and 0.1-6% of those will develop dysphagia. (3) Dysphagia from hyperostosis is most commonly associated with anterior osteophyte formation of C3-C5, likely due to the fact that the normal epiglottic tilt lies over the laryngeal inlet at this level. (19) However, cases of dysphagia have been reported to occur due to protrusion in the thoracic regions as well. (14) In this present case, cervical vertebral bodies were fused by bridging of the anterior osteophytes that resulted from the ossification of the anterior longitudinal ligament from C2 to C5. The most likely mechanism of dysphagia would be its interference in swallowing in the pharingoesophageal junction, although osteophytes in the lower cervical spine can also interfere with esophageal peristalsis. (5) Several mechanisms have been described whereby an osteophyte can generate dysphagia. Firstly, a large osteophyte may cause direct mechanical obstruction of the esophagus or hypopharynx. Secondly, dysphagia may be caused by small osteophytes, if they are located at fixed points in the esophagus (cricoid cartilage at level C6). Thirdly, osteophytes may cause an inflammatory reaction around the esophagus or a compression neuropathy. (5) In our case, the cause was mechanical compression of oesophagus by large osteophyte anterior to C2 and C3 vertebral bodies. The diagnostic imaging approach should include a lateral X-ray, barium swallow, and CT. The formation of an osteophyte, the degree to which it compresses the esophagus, and its extent (craniocaudal and anteroposterior) can be demonstrated by plain lateral radiographs, barium swallow, and CT, respectively. (7) Magnetic resonance imaging (MRI) may also be considered in patients with additional symptoms, such as dyspnea and dysphonia, to identify any soft tissue damage, perforations, or superinfection. MRI is also useful to evaluate any concomitant central or foraminal cervical stenosis that the surgeon may wish to address at the time of osteophytectomy. (7) Patients should undergo an appropriate ENT and endoscopic examination. The treatment of dysphagia as a result of cervical hyperostosis in the context of DISH is conservative or surgical. Patients who have minimally bothersome symptoms should be treated with conservative methods, such as dietary modifications, a swallowing therapy and a prescription of non-steroidal anti-inflammatory drugs in the early stage. (2) Where conservative management fails to control symptoms or weight loss is observed, surgery may be considered. The literature suggests that osteophyte resection is considered to be highly successful when conservative methods fail. (4,8,11,13,18,) Resection should be performed through an anterior route with the usual approach, resecting the osteophyte with a chisel, rongeurs or drill. However, one must be careful while excision of the osteophyte as the pharyngo-oesophageal segment may be adhered to the osteophyte and requires meticulous blunt dissection prior to excision otherwise, there may be oesophageal injury. The osteophytectomy without spinal fusion is advantageous due to no implant-associated complication and less operation time. However, recurrent formation of the osteophyte may occur. The recurrence rate for the osteophyte is unclear, but there are some reports that the presence of postoperative intervertebral mobility was found to be a significant risk factor in the recurrent formation of osteophytes. (11) CONCLUSION DISH is a common cause of the anterior cervical osteophyte resulting in the progressive dysphagia. This clinical entity should be included among the differential diagnoses of dysphagia in elderly adult patients. Patients with significant symptoms who fail conservative management should be considered for osteophytectomy. Outcomes following osteophytectomy are very favorable. Conflicts of interests: The authors declare that they have no conflicts of interest concerning this article. Authors’ contribution: All the authors had contributed to this manuscript.
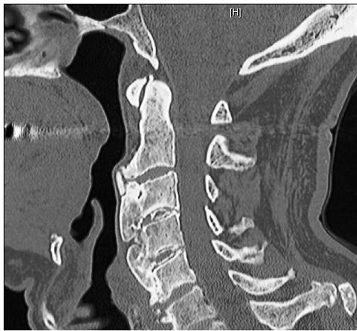 Figure 1: Sagittal CT image of the cervical spine showing large anterior osteophytes extending from C2 to C5.
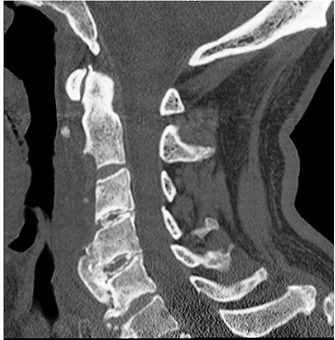 Figure 2 : Postoperative sagittal CT image of the cervical spine confirming successful removal of the C2 to C3 and C3 to C4 osteophytes. REFERENCES
|
© 2002-2018 African Journal of Neurological Sciences.
All rights reserved. Terms of use.
Tous droits réservés. Termes d'Utilisation.
ISSN: 1992-2647