
|
|
|
CASE REPORT / CAS CLINIQUE
CASE REPORT: CALCIFIED CHRONIC SUBDURAL HAEMATOMA IN AN ELDERLY NIGERIAN
HEMATOME SOUS DURAL CHRONIQUE CALCIFIE CHEZ UN NIGÉRIAN ÂGÉ. A PROPOS D'UN CAS
E-Mail Contact - BANKOLE Olufemi Babatola :
f_baba@yahoo.com
ABSTRACT Calcified chronic subdural haematoma [CCSDH] is a rare complication of the relatively more common condition of Chronic Subdural Haematoma (CSDH). We present the case of a 68yr old man referred with a 2 week history of sudden onset Right hemi paresis generalized tonic clonic seizures and aphasia. There was a history of mild head injury 7 years prior to presentation and computerized tomographic scan showed features suggestive of a Calcified Chronic Subdural Haematoma. He deteriorated rapidly prior to surgical intervention and had an emergency craniotomy with evacuation of the lesion performed. Unfortunately patient died 12 hours post operatively never having woken up after the operation. An acute subdural haematoma was discovered at post mortem. Keywords : armoured brain, calcified chronic subdural haematoma. RESUME L’hématome sous-dural calcifié (HSDCC) est une complication rare Nous présentons le cas d’un patient de 68 ans ayan présenté en deux semaines une hémiparésie avec des crises toniques généralisées associée à une aphasie. Les antécédents étaient marqués par une blessure légère de tête 7 ans auparavant. Le scanner a montré des images suggestives d’hématome sous-dural calcifié. Il s’est détérioré rapidement avant l’intervention chirurgicale et a eu en urgence une craniotomie avec évacuation de la lésion. Malheureusement le patient est décédé 12 heures après l’opération sans s’être réveillé. L’ HSDCC a été découvert en post mortem. Mots clé : Hématome sous dural , Hématome sous dural chronique, calcifié. INTRODUCTION Calcified chronic subdural haematoma [CCSH] is an infrequent complication of the more common condition of Chronic Subdural Haematoma(7,8,9). Since it was first described in 1884(7), many reports have been generated especially with the advent of modern neuroimaging. The diagnosis is usually made with the aid of a CT scan or an MRI although a plain skull X-ray will also show the calcific density. These calcifications are mostly found at the convexities(17,2,10,18,13,15,11). While there are many reports in literature highlighting this condition no previous report of this condition in our environment exists even though subdural haematoma is well recognized. CASE SUMMARY A 68yr-old man was referred for Neurosurgical review on account of Brain CT scan findings. He had a 2-week history of sudden onset of weakness of the right side of the body, loss of speech and generalized tonic clonic seizures. There was no associated loss of consciousness. He regained speech later but it remained slurred. There was a history of mild head injury 7 years prior to presentation. He was not a known hypertensive or diabetic. He was being treated for a presumed Cerebrovascular Accident (CVA) when a Brain CT scan was done and he was sent for Neurosurgical review. DISCUSSION Calcified chronic subdural haematoma was first described in 1884(7,1) as a postmortem finding and is found in 0.3 – 2.7% of patients with chronic subdural haematoma(8,9,3). It occurs more frequently in children and young adults than in the elderly(3). It is sometimes referred to as armoured brain’. The pathogenesis of CCSH is unclear, the haemorrhage is thought to progress from hyalinization to calcification but it has been found that it takes at least six months for calcification to develop. However cases have been reported occurring many years after initial trauma as in our patient who became symptomatic seven years after the head trauma. (13,1,3,12). Patients can present with hemiparesis, aphasia, seizure, gait disturbances, mental and physical retardation and altered consciousness(17). However asymptomatic cases have also been reported(12,6). Other conditions that can be considered to mimic CCSH are calcified epidural haematoma(18), calcified chronic subdural empyema(5), meningioma(2), and calcified arachnoid cyst(15). Treatment of CCSH depends on whether it is asymptomatic and also the age of the patient. Some workers have advocated observation for elderly patients with little or no symptoms. However, most surgeons agree that the onset of acute symptoms related to the lesion should be treated by craniotomy and excision of the organized clot. Sometimes the inner membrane is adherent to the underlying brain but this can usually be separated from the underlying arachnoid although this was not possible in our patient. Generally good post operative neurological recovery is reported in most cases with gradual but definite improvement in pre operative clinical state. Acute subdural haematoma is a known complication following surgery and it could be fatal as seen in this case. Our patient showed a rapid decline in his clinical condition over a relatively short period of time. The poor outcome from surgery can be attributed to the significantly altered level of consciousness by the time of intervention. CONCLUSION Calcified chronic subdural haematoma is a rare but treatable condition. Modern imaging techniques have made its diagnosis easier and removal of the mass lesion when indicated is achievable. Acute subdural haematoma is a recognized post-operative complication and this can be fatal if not diagnosed early and treated promptly. Delay in intervention after onset of symptoms can result in a poor outcome. 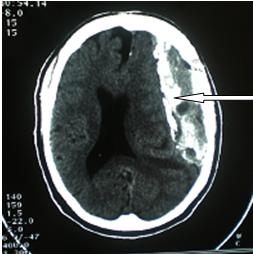 Figure 1  Figure 2 REFERENCES
|
© 2002-2018 African Journal of Neurological Sciences.
All rights reserved. Terms of use.
Tous droits réservés. Termes d'Utilisation.
ISSN: 1992-2647