CASE REPORT / CAS CLINIQUE
SPINAL METASTASIS FROM A GROWTH HORMONE PRODUCING PITUITARY TUMOUR
- African Neurological Diseases Research Foundation, Nairobi, Kenya
E-Mail Contact - OLUOCH-OLUNYA D. :
SUMMARY
We present a case of a growth hormone secreting pituitary adenoma with successive spinal cord metastasis at 6 and 11-year interval following craniotomy and radiotherapy. The lesions were cervical, thoracic and cauda equina and were successfully surgically removed. The MRI and histological findings are discussed and the literature reviewed.
Keywords : Pituitary, Metastasis, Spinal
RESUME
Les auteurs rapportent un cas d’adenome de l’hypophyse secretant avec des metastases medullaires survenues 6 ans et 11 apres la craniotomie et la radiotherapie. Les lesions medullaires cervicales, dorsales et de la queue de cheval ont ete operees avec succes. Les aspects neuroradiologiques, histologiques, et une revue de la litterature font l’objet d’une discussion.
INTRODUCTION
Subarachnoid dissemination (1,2,3,4) local invasion and haematogenous spread of pituitary adenoma are recognised presentations though it continues to be one of the most benign tumours of the central nervous system (CNS)6. Varied reports have not shown any preponderance to the histological type (7, 8, 9), non-secreting, prolactinomas, and growth hormone secreting tumours. Intracranial deposits have been reported more frequently 2 and have been managed by local excision where feasible, disseminated disease though is notoriously refractory to treatment dopamine agonists. spinal irradiation, interferon and chemotherapeutic agents have all been tried.
CASE REPORT
1st Admission
In December 1988 at the age of 45 years our patient presented with gradual visual loss and increase of his hand and feet size. A CT scan carried out in Kenya had shown a large pituitary mass. He was referred to the National Hospital for Nervous Disease Queen’s Square London where he was noted to be diabetic requiring insulin for control. A craniotomy and decompression of a somatotroph adenoma was carried out followed by conventional radiotherapy. His vision markedly improved and was left with a minimal restriction of his right temporal field. The insulin requirements also tailed off completely post operatively.
2nd Admission
At 51 years, he represented in November 1994 to Frenchay Hospital Bristol (U.K.) with a progressive lower motor neuron weakness of the left upper limb and a partial Brown Sequard myelopathy causing right lower limb sensory loss and left lower limb pyramidal weakness. Baseline pituitary tests showed a low random cortisol and growth hormone of 22ng/ml. MRI showed three IDEM lesions at C3/4, C4/5 and C7/T1 which were excised. Histology confirmed metastatic growth hormone secreting tumours.
3rd Admission
At 56 years, he presented in September 1999 to the Nairobi Hospital with a 6 month history of increasing recumbent back pain radiating to his left lower limb with attendant bilateral weakness of his ankles. He was ambulant with the use of a stick and had bilateral foot drop; the power was 2/5 MRC left and right respectively. He had erectile dysfunction but no incontinence of urine or stool. MRI of the thoraco-lumbar Fig (1) region showed an intradural extramedullary tumour (IDEM) T12 to L2. He also had a coincidental disc protrusion at L5/Sl. A thoraco-Lumbar laminectomy was carried out and a 3x4x6cm red triable tumour, which was covered by the nerve roots, was excised in total. Histology confirmed metastatic pituitary tumour. His back pain settled well, there is some residual weakness ofdorsiflection on the left which we expect to improve further and he is now ambulant without the use of a stick.
DISCUSSION
Metastatic pituitary tissue with endocrine function is rare. Biochemical cure following complete surgical resection of spinal canal metastasis lias been described once previously as. The same patient has represented 6 years later in his home country Kenya with a histologically begign tumour in the cauda equina. The patient has survived 12 years since the first onset of symptoms and to date has no evidence of intracranial recurrence of tumour. A mean survival time of 5 years (range of 20 days to 12 years) has previously been reported (2). MRI scanning following resection of lesions in his cervical spine in 1994 did not reveal any other macroscopic deposits in the neuro-axis. Correlation between histological type and preponderance to metastasise has been poor 4,5,1 l,l2 several reports like ours show a histologically begign ‘metastatic’ lesions. Metastasis within the neuroaxis is thought to be via Subarachnoid and haematogenous spread. Surgical intervention within the basal cisterns has been implicated in the potential lor subarechnoid dissemination. Lumbar CSF examination confirming the presence of tumour cells has also been used previously 2. A new histological technique, proliferating cell nuclear antigen (PCNA) has been developed to predict local recurrence in adenomas of the pituitary (13) . This has been used lo determine the proliterative potential of a classic pituitary adenoma which 1’netastasiscd intracranially and has been used to predict aggressiveness of the tumour 14 with variable results.
The question of radiation to the tumour remnant being carcinogenic to a previous benign tumour has been deemed as uncommon (15).
The management of metastatic pituitary adenoma remains poor: dopamine agonists have been used in the treatment of prolactinomas and somatotrophic tumours (16,17). Whole spine radiation in four parts lias also been used to control spinal dissemination (2) with initial reduction of intracranial and spinal tumour size, there was subsequent regrowth of tumour with fatal consequences.
CONCLUSION
This is the first case reported in the literature of successive intraspinal growth hormone secreting pituitary adenoma adequately treated by surgical excision. We feel that he is also unique in that he has presented to several units in two continents with good cros references. Metastatic pituitary adenoma though are has such a poor prognosis as to whether consideration for spinal CSF cytology, hormone levels, PCNA analysis of the tumour for reactivity should be done to enable us to predict the cases that are likely to progress.
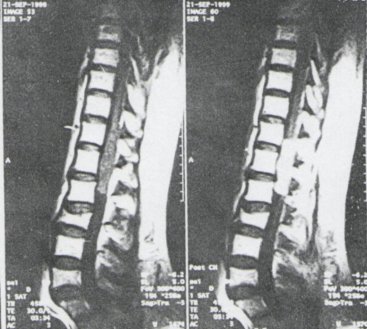
Figure 1
REFERENES
- NELSON PB, ROBINSON AG, MARTINEZ AJ, Metastatic tumor of the pituitary gland: Neurosurgery 1987 Dec;21 (6): 941-4.
- PLANGGER CA. TWERDY K, GRUNERT V, WE1SER G, Subarachnoid metastases from a prolactinoma: Neurochirurgia (Stuttg) 1985 Nov; 28 (6): 235-7
- OGILVY KM, JAKUBOWSKI J, Intracranial dissemination of pituitary adenomas: J Neural Neurosurg Psychiatry 1973 Apr;36(2): 199-205
- KUROKI M, TANAKA R, YOKOYAMA M, SH1MBO Y, Ikuta, Subarachnoid dissemination of a pituitary adenoma: Surg Neurol 1987 Jul; 28 (I): 71 -6
- SANG H, JOHNSON C. Metastatic prolactin secreting pituitary adenoma. Hum Pathol 1984; 15:94-6
- HASHIMOTO N, HANDA H. NISHI S. Intracranial and Intraspinal dissemination from growth hormone secreting pituitary tumour-Case report: JNciirosiirg 1986 Jan; 64:140-144
- TAYLOR WA, UTTLEY D. WILKINS PR, Multiple dural metastases from a pituitary adenoma. Case report. :J Neurosurg 1994 Oct; 81 (4): 624-6
- ROCKWELL BH, PICA R, RAJ1 MR. DASTUR KJ. ALTSCHULER EM, JOHNSTON JM Intrathecal metastatic pituitary prolactinoma: AJRAm JRoentgenol 1996 Nov: 167(5): 1295-6
- SAKAMOTO T, 1TOH Y. FUSHIMl S, KOWADA M. SAITO M, Primary pituitary carcinoma with spinal cord metastasis – case report.: Neural Med Chir (Tokyo) 1990 Oct: 30(10): 763-7
- DAYAN C, GUILDING T. HEARING S. THOMAS P, NELSON R, MOSS T, BRADSHAW .1. LEVY A, LIGHTMAN S, Biochemical cure of recurrent acromegaly by resection of cervical spinal canal melastases. : Clin Endocrinol (Oxf) 1996 May; 44 (5): 597-602
- MASONIC MJ, RUBENSTEIN LJ DASCO MR et al: Chromophobe adenoma of pituitary gland with Subarachnoid metastasis. Neurology 1963; 13:836-40
- EPSTER1N JA, EPSTE1N BS. MOLHO L, ZIMMERMAN HM. Carcinoma of the pituitary gland with metastasis to the spinal cord and roots of the cauda equina.J Neurosurge 1964; 3 1:846-53
- HAO DW, HAKIM F, B1LLER BM etal. Significance of proliferating cell nuclear antigen in predicting pituitary adenoma recurrence. .J Neurosurg 1993:78: 753-6
- O’BREIN DP, P111LL1PS JP, RAWLUK DR. PARREL MA. Intracranial metastasis from pituitary adenoma. Br .J Neurosurg 1995 ;9: 21 I -21 8
- LANDOLT AM: Ultrastructure of human sella tumours. Malignant pituitary tumours. Ada Neurochir Suppi 1975;22:94-103
- LUIZZ1 A, CHIODONI PG, BOTALLA L. et al: Decreased plasma growth hormone (GH) levels in acromegalics following CB 154 (2-Br-o-ergocryptine) administration. J Clin. Endocnnol Mctub 1974; 38:910-912,
- WASS JAH, THORNER MO, MORRIS DV et al: longterm treatment of acromegaly with bromocriptine. Br Med .J 1977:1875-878