
|
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|
ORIGINAL PAPERS / ARTICLES ORIGINAUX
FATAL NON- TRAUMATIC INTRACEREBRAL HAEMORRHAGE SECONDARY TO HYPERTENSION: A TEN- YEAR RETROSPECTIVE AUTOPSY STUDY.
HÉMORRAGIE INTRACÉRÉBRALE MORTELLE NON-TRAUMATIQUE SECONDAIRE À L'HYPERTENSION : UNE ÉTUDE RÉTROSPECTIVE DE DIX ANS D'AUTOPSIE.
E-Mail Contact - SOKUNLE Soyemi Sunday :
soyemisunday@yahoo.com
ABSTRACT Background and purpose: Worldwide, stroke is the second most common leading cause of death and also one of the leading causes of disability. In the last decades, more studies have focused on ischemic stroke. This study focused on intracerebral haemorrhage which is a common subtype of stroke. Method: This is a -ten year retrospective study of all autopsies with cases of intracerebral haemorrhage following hypertension as cause of death. The age, sex, anatomical location of the bleeding and any ventricular extension were extracted from the autopsy register. The data were analysed using the statistical package for social science (SPSS) Software version 18. Results: There were 397 cases of intracerebral haemorrhage with age ranging from 16 and 85 years. The mean, mode and median ages were 50.45±12.47, 50 and 50 years respectively. There were 272 (68.5%) males and 125 (31.5%) females with a male to female ratio of 2.2:1. Age group 41 – 50 years has the highest prevalence, while the least value (5.3%) was seen for the 70 years and above. The most common site of bleeding was the cerebral hemisphere with 88% having ventricular extensions. This study revealed that hemispheric haemorrhage occurred in approximately three out of every four haemorrhagic strokes. Conclusion: Hemispheric haemorrhage is the most common site of bleeding in this study, the majority of which are complicated by ventricular extension. The male sex is twice more affected than the females and the highest occurrence is seen in males in the 41-50 years age group. Keywords: cerebrum, bleeding, brainstem, cerebellum, intracerebral haemorrhage, ventricle INTRODUCTION Spontaneous non-traumatic intracerebral haemorrhage is bleeding into the parenchyma of the brain with occasional extension into the ventricles and rarely into the subarachnoid space [22]. It commonly occurs in the lobes of cerebral hemispheres, basal ganglia, thalamus, brain stem and cerebellum.[17] If the haemorrhage occurs in the basal ganglia and thalamus, this is designated ganglionic haemorrhage while those that occur in the cerebral lobes are called lobar haemorrhages [24]. This haemorrhage could also either be primary or secondary depending on the underlying cause of the bleeding. Those due to hypertension following damage to the small vessels or amyloid angiopathy are referred to as primary haemorrhage while other causes such as tumour, defective coagulation or arterio-venous malformations are referred to as secondary intracerebral haemorrhage [11] Globally, the incidence of intracerebral haemorrhage varies from 10 to 20 cases per 100,000 population and increases with age as previously reported by various studies. [4,12,13]. This incidence is however, higher in Blacks (up to 50 per 100,000) and is twice the incidence in Whites.[23] The haemorrhage occurs in middle age to late adult life with peak incidence at about the age of 60 years [24]. Other studies have also revealed it to be more common in men than women especially those older than 55 years [13,26]. It is a clinically significant cause of morbidity and mortality. In the light of the aforementioned and considering the fact that there is paucity of autopsy studies on this subject especially in Africa. The aim of this study is to examine the epidemiological and morphological features in cases of spontaneous non- traumatic intracerebral haemorrhage secondary to hypertension at post mortem examination. MATERIALS AND METHODS This is a -ten year (January 2006 to December 2015) observational retrospective study of all autopsy cases of intracerebral haemorrhage following hypertension seen in the Department of Pathology and Forensic Medicine, Lagos State University Teaching Hospital, Ikeja, Lagos, Nigeria. The department conducts autopsy services for the teaching hospital as well as coroner’s autopsy for the state. During post mortem examinations, the skull is opened and brain is removed in all cases. The age, sex, anatomical location of the bleeding and any ventricular extension is noted. All these were recorded in a pre-designed data collection form. The data were retrieved from the autopsy reports and analyzed using the Statistical Package for Social Science (SPSS) Software version 18. The data were presented in tables, percentiles, pie chart and bar chart. Test for significant was set at P< 0.05. RESEARCH MATERIAL Approval from the Department of Pathology and Forensic Medicine of Lagos State University Teaching Hospital, Ikeja was sought and received before the study could be done. Materials used include the autopsy register, post mortem reports, and clinical notes where applicable. STUDY POPULATION Lagos State University Teaching Hospital (LASUTH), Ikeja is one of the tertiary health care institutions located in the South Western geo-political zone of the country, serving a core population of approximately seventeen (17) million people of diverse backgrounds.[21]. All cases of intracerebral haemorrhage resulting only from hypertension were used in this study. The diagnosis of hypertension at post mortem examination was made based on the following criteria. Heart weight in excess of 300gm for females and 350gm for males; left ventricular wall thickness of more than 1.5cm taken at a point 1-2cm below the mitral valve and papillary muscle thickness of more than 1.5cm.Any other causes of ventricular hypertrophy such as aortic stenosis were excluded. It includes all ages and sex. All embalmed bodies with intracerebral haemorrhage were also included. Thirty five cases with advanced decomposition and who had subarachnoid haemorrhage from aneurysmal rupture or any other causes were excluded. Also excluded were cases of intracerebral haemorrhage not caused by hypertension such as coagulation disorders, tumours, arteriovenous malformation and illicit sympathomimetic drugs (amphetamine or cocaine overdose). RESULTS There were a total of 397 cases of ICH with evidence of hypertensive heart disease. The age range in this study was 16 to 85 years. The mean, mode and median ages were 50.45±12.47, 50 and 50 years respectively. There were 272 (68.5%) males and 125 (31.5%) females with a male to female ratio of approximately 2.2:1. See Table 1. Age classification was done in decades starting from below 30 years to 70 years and above age groups. The highest value of 116 (29.2%) was seen in age groups 41 – 50 years, this was closely followed by 51 – 60 years age groups representing 109 (27.5%) while the least value of 21 (5.3%) was seen for the 70 years and above age groups. The most common site of bleeding was the cerebral hemisphere which accounted for 292 (73.6%). The second most affected part of the brain was in the pontine region representing 76 (19.1%) while cerebellar haemorrhage accounted for 29 (7.3%). This study revealed that hemispheric haemorrhage occurred in approximately three out of every four haemorrhagic stroke. (Table 1). Among those post mortem with bleedings into cerebral hemisphere a total of 88% had ventricular extension. See Figure 1. Table 4 also revealed P value of 0.389, this implies that the hemorrhage affected all the parts of the brain equally across the age groups. DISCUSSION Worldwide, stroke is the second most common leading cause of death and also one of the leading causes of disability [7,19]. That its burden will most likely increase in developing countries has been corroborated by previous works [1, 27]. In the last decades, a lot of progress has been achieved in the etiology and management of stroke although; most studies have focused on ischemic stroke [14]. This study focused on intracerebral haemorrhage which is a common subtypes of stroke and constitutes 10-20% of all strokes globally and 20-30 % in Africa [6, 8]. To the best of our knowledge there is no other post mortem series on stroke secondary to hypertension published from Nigeria and the rest of Africa. The available data on intracerebral haemorrhage has been deduced from African American and the Caribbean.[9,16,3] Our study revealed that intracerebral haemorrhage from hypertension occurred twice as common in males than females. The highest incidence also occurred in the 41-50 year age group. These two findings are consistent with a clinico-pathological studies on cerebrovascular accidents done in Ibadan, Western Nigeria by Osuntokun et al [20]. In their study, the peak incidence was in the age group 40-49 years with male to female ratio of 1.7 to 1. It is also supports and consistent with the findings of Ezeala- Adikaibe in South Eastern Nigeria [5] in which ICH was diagnosed from all the CT scan over a period of 11 years. Their study revealed male to female ratio of 2 to 1 with a mean age of 58.8 years; lobar and deep cerebral haemorrhage peaked at 16-39 and 40-49 years respectively. It is also worthy of emphasis, that peak age of incidence of ICH in our study was 41-50 years. This is in agreements with the study in Nigeria by Ezeala- Adikaibe in South Eastern Nigeria [5].This revelation is not surprising considering the sedentary habits, drug use, alcohol consumption, smoking and eating habits of people in this age groups who are The glaring predominance of hemispheric haemorrhage as the overall most common ICH sites in our study is corroborated by previous works in Mexico by Ruiz-Sandoval et al [25], USA[9], France [13]Sweden [18], Japan [15], Finland [10] and Australia.[2]. However, this is in contrast with the findings in a large population-based study in Japan [15] where it accounted for only 15%, while putamen was the most common (34%). The reason for this could be a subject for future study. In most populations [13, 9, 25, 18, 15, 10,] incidence of cerebellar haemorrhage is usually higher than pontine haemorrhage. These findings are however at variance with our results where this was the reverse except in the 41-50 and 61-70 age groups. Again, our work was an autopsy based study while others were clinically based suggesting that more deaths resulted from pontine haemorrhage. This finding could be due to high incidence of hypertension in the former and the likelihood of high occurrence of amyloid angiopathy in the latter groups. An interesting finding is the very small percentage of ventricular extension reported in a previous study in Eastern Nigeria.[5]. This is in contrast to our study which revealed a predominant ventricular extension. The previous study made their diagnoses on CT scan, there was a possibility of missing out some of the ventricular extensions especially if enough slices were not made. In addition, many patients may likely survive if the ventricular extension is minimal, while majority will be fatal if the extension is massive. The latter could have accounted for the predominant percentage since it was an autopsy based study CONCLUSION Hemispheric haemorrhage (Deep and Lobar haemorrhage) most of which are complicated by ventricular extensions is the commonest site of bleeding in this study. Frequency in males is twice that of the females while the highest occurrence is seen in males in the 41-50 years age group.This study revealed that hemispheric haemorrhage occurred in approximately three out of every four haemorrhagic strokes. Financial Support and Sponsorship. Nil Conflicts of interest There are no conflicts of interest Author’s contribution SSS is a Lecturer and Consultant Pathologist who was responsible for the conceptualization, design of the study and did the literature search. FFA is a Senior Lecturer who contributed to the literature search and did the critical review of the article for intellectual content. OOO and SDA are consultant pathologists who analyzed the data while WOO is a senior registrar who collected the data. All authors read through the draft and approved for publication. Table 1. Table showing the gender, age and site of bleeding distribution (n=397)
Table 2: Table showing the distribution of sex with age groups. (n=397)
P= 0.289 Table 3: Table showing sex distribution with site of bleeding. (n=397)
P= 0.771 Table 4: Table showing age distribution with site of bleeding. (n=397)
p=0.389 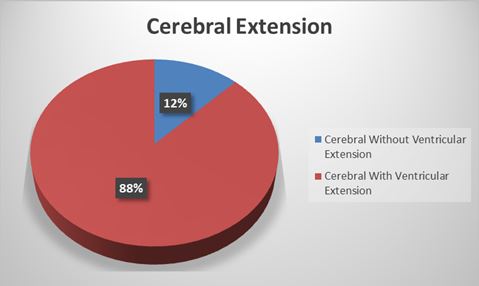 Figure 1 REFERENCES
|
© 2002-2018 African Journal of Neurological Sciences.
All rights reserved. Terms of use.
Tous droits réservés. Termes d'Utilisation.
ISSN: 1992-2647