
|
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|
SUMMARY Hospital-based data on neurological disorders from Mahajanga, the Northwestern province of Madagascar are reported. RESUME Les auteurs rapportent les donnees hospitalieres sur les troubles neurologiques rencontres a Mahajanga, province occupant la partie Nord-ouest de Madagascar. Les epilepsies (28,75% des cas), les cephalees chroniques (20,95%), les neuropathies peripheriques (11,30%) constituent les affections les plus frequentes. Contrairement aux statistiques occidentales, les maladies degeneratives et la sclerose en plaques sont rares. Les principaux facteurs de risque (maladies transmissibles, manultrition, stress provoques par la pauvrete) et quelques aspects des realites sanitaires (manque d’equipments de diagnostic et de medicaments fondamentaux) sont partages avec d’autres pays tropicaux en voie de developpement. Keywords : Epidemiology, Neurological diseases, Madagascar INTRODUCTION Tropical countries share common climatic and biologic characteristics. They are thus expected to disclose similar patterns of diseases. However, the prevalence of these diseases vary because of the development and of the sociocultural peculiarities of each country. Population-based studies, the most appropriate ones to assess the magnitude of each health problem are unavailable in Madagascar. We report hospital data from Mahajanga, a Northwestern region of the island. STUDY POPULATION AND METHOD The study population was expected to be that of the whole province (1,379,000 inhabitants), but in fact, only the population of the city of Mahajanga and its nearest surroundings (up to 200,000 inhabitants) had access to the University hospital. The population was young (44<15 years-old, only 3,2°/o>65 years-old), with an isosexual repartition expectancy (52 years vs 69 years for Mauritius) [1]. A considerable proportion of Mahajanga city dwellers have an Islamic influence, expressed in prohibitory eating behaviours (pork, alcoholic, drinks). The region has a hot and dry climate where malaria, schistosomiasis tuberculosis and syphilis are endemic. The study itself consisted in a retrospective exam of registered inpatients and outpatients’ files in the department of Neuropsychiatry (University Hospital) between June 1, 1993 and December 31, 1995. Patients of both sexes, aged more than one year-old were included. Electrical devices (EEG.EMG), cerebral imageries (CT scan, MRI), and sophisticated biological investigations were unavailable, so the diagnosis was built up on sole clinical and routine laboratory data. In fact, the most conclusive argument was the radical cure or alleviation of symptoms. The classification of the diseases was made according to internationally.recognised definitions (NINDS, IHS, ILAE, ICD 10). RESULTS 1161 patients were registered during the study period: 741 had neurological disorders, 334 had psychiatric disorders, 86 had non neuropsychiatric diseases (table 1). Table 1: Repartition of the diseases registered at the Departement of Neuropsychiatry during the study period.
Outpatients represented 68,42% of cases (n=507) and inpatients 31,58% of cases (n=234). Epilepsie were followed by chronic headaches, which were selectively recruited among outpatients, cerebrovascular diseases occupied the second place among inpatients; the real magnitude of this affection might be underevaluated, because of parallel recruitment in other wards. Unlike series from industrialised countries, degenerative diseases were rare. Peripheral neuropathies were common, whereas spastic paraparesis were of a minor concern. Two per cent (2%) of neuropathies (15/741) were inclassifiable because of tlie lack of specific investigations. Table 2: Aetiological repartition of the neurological disease (in percentage) among all the patients, outpatients and inpatients.
Epileptic seizures were listed in table 3: their classification, according to the 1981 ICE version was possible in spite of EEC data unavailability. Some authorities have admitted the validity of such classification (2,3). Like in most of tropical reports (3,4,5), partial seizures were predominant wheras absence seizures were underrated (1% vs 10% for GASTAUT’s [6]. Among the epilepsies which were deemed as secondary (56%=l 19/213), a putative aetiology was found in only 54% of them (64/119). Neurocystcercosis was the commonest pathology involved (42% of the aetiologies, i.e. 27/64). Phenobarbital was the drug of first choice (94% of the prescriptions). The other antiepileptic drugs were either unavailable, or too expensive. Table 3: Distribution of the epileptic seizures according to the international Classification (ICES), 1981 version.
Chronic headaches were dominated by migraine (table 4); tension headaches were unexpectedly rare. Many physicians were still unfamiliar with migraine, as judged by the non negligible rate of diagnosis wanderings (spasmophilia, ocular dsyfunctions, sinusitis), and maladjusted prescriptions (preventive treatment prescribed for one month.). Long term management of migraine suffered from the same bad compliance than that encountered in epilepsies; the main reasons were unavailability or cost inaccessibility (in percentage). Table 4: Aetiological repartition of the chronic headaches (in percentage).
The aetiology investigations and the classification ofneuropathies (table 5) were limited by the lack of diagnosis facilities (EMG, nerve conduction studies, specific biologic dosages). The main putative cause asserted was polyvitamins deficiency (26% of cases, ie 27/102) within the frame of global malnutrition or alcoholism. Heavy deficiency sufferers (e.g prisoners) sometimes disclosed aproximal hindlimbs involvement. Three cases were associated with heart failure (wet beriberi). Radicular compressions (mainly of the sciatic type) were surprisingly overrepresented in our series, whereas facial nerve palsy was unfrequent (8,82% of cases). Unlike some African countries (7), no HIV-related palsies were encountered. Mahajanga has a leprosarium, so only a typical manifestations of this infectious disease were addressed in our department (2,94% of cases). Table 5: Repartition of the different anatomoclinical forms of neuropathies (in percentage).
Like in the majority of Caucasian (8) and African studies (9,10), strokes were dominated by the ischemic type (table 6). Table 6:
Hypertensive encephalopathy was screened with accuracy because of its better therapeutic issue. Hypertension and syphilis were the main risk factors identified. The global fatality rate was high (58% of cases, i.e. 48/83). Neurosisticercosis was at the head of CNS infections (table 7), although the anatomical specimen prevalence of this Parasitosis (II) was among the lowest in Mahajanga.(6°/o vs 40% for Antananarivo, 32% for Tulear, 15% for Fianarantsoa). Diagnosis was made on sole clinical and serological basis (12); in fact, the therapeutic trial remained the most conclusive argument. Bacterial infections of the cerebrum and its coverings were surely underestimated because of parallel recruitments. Table 7: Frequency of CNS infections (in percentage).
Intrathecal antibiotics were often useful to palliate the dose inadequacy of parenteral drugs. Cerebral malaria, like in the other underdeveloped countries (13), provided a high fatality-rate (26% of case, ie 4/15), because of delayed chemotherapy. Neither HIV carriers nor proved quinine resistance was encountered among our fatal cases. Among degenerative affections. Parkinson’s disease was the most frequent. Parkinsonism related to chronic use of neuroleptics was far commoner. Alzheimer-type dementia was not yet a public health problem. DISCUSSION The data from Mahajanga, globally display the same patterns of neurological diseases as those found in the majority of tropical regions. In spite of the lack of population-based studies, the leading position of epilepsies among our hospital-registered cases confirm their importance in public health. The predominance of partial seizure parallels the high rate of secondary epilepsies. However, their pattern is not homogenous in different tropical countries: Nigerian studies (4) emphasize the causative role of febrile convulsions to explain the higher rate of complex partial seizures; on the contrary, Indian studies (5) yield a higher rate of partial simple seizures (58% of cases) and credit the prominent role of CNS infections, amongst which neurocysticercosis is paramount. Our pattern is of the Indian type (table 3) and this parasitosis, really plays an important role. Additional studies on risk factors, appropriate drug supply (14/15) and pertinent education of the population, are the most adapted means to fight against epilepsies. Concerning chronic headaches, post graduate training is needed to improve the diagnosis and the management of the main aetiologic forms, viz migraine and headaches of psychological origin. Drugs availability and cost must be taken into account in case of long term treatment; patients compliance depend on these extramedical factors. Traditional pharmacopoeia (16) and alternative medicine (17) are optional or complementary issues for developing countries, but their use must be regulated. Peripheral neuropathies are probably underrated, for a bulk of patients to the hospital recruitment; the reasons may be a self management with vitamin and plants, geographical isolation and so on. The endowment of essential facilities (EMG, nerve conduction measurement, biological dosages) will enrich the knowledge about these diseases, common in tropical countries; certain aetiologies are likely different from those encountered in Western regions. Massive polyvitamins deficiency is frequent among prisoners. Associated with a major protein calorie malnutrition it can provoke both axonal and segmental demyelination (18); this latter may explain the involvement of proximal hind-limbs in many patients. It is surprising to detect HTL V1 among Malagasy patients, for the Seychelles, which share the same climatic, ecological, and even cultural characteristics with Madagascar, are considered as endemic areas The surprising high rate of nerve sciatic compression results likely on local inadequacy in professional training: indeed, Mahajanga is a port, and naive load handlers are recruited without any technical skill learning. However, lumbar disk prolapse is considered as a rather rare condition in Africans (20). Although the proportion of our stroke cases represent only one-third of those reported in the majority of African hospital-based studies (9,10,21,22), they constitute a real human and economic burden; the lack of appropriate diagnosis and therapeutic supplies may explain the high mortality rate, and the worse functional prognosis. Global campaign against hypertension, the main risk factor, has proved to be an efficient method to decrease the secular trend of strokes (23,24). The infection of the CNS are by far the most important causes of mortality and mobidity in many African countries (25). Our data, probably underestimate their real importance, because of parallel recruitments. The prognosis is often worsened by the delayed management and by the incapacity in identifying and treating adequately the infectious agent. Like in other African series, degenerative diseases are rare, independently of the low life expectancy (26). Before concluding on a case of AIzheimer’s disease, tertiary syphilis and major depression must be ruled out. CONCLUSION The patterns ofneurological diseases in Mahajanga (Madagascar) are globally similar to that of the majority of tropical countries. A descriptive epidemiological survey on general population and epidemiological research on risk factors are basic to build up an appropriate preventive policy. Without an endowment of essential diagnosis facilities (EEG, EMG, Echography) and drugs, curative care would be inefficatious; this failure will reinforce the negative attitude of the population towards Western medicine and favour the action of quacks. PITUITARY ABSCESSSUMMARY Pituitary abscess is a rare disease that remains very difficult to diagnose preoperatively even with newer imaging techniques such as CT – and MRI scanning. We describe four cases, of which only one was diagnosed pre-operatively. Pituitary abscess may present as meningitis in a patient with enlarged sella on skull x-rays. More commonly it is indistinguishable from a pituitary tumour both clinically and radiologically and the diagnosis comes as a surprise at surgery. Treatment is by transsphenoidal drainage, appropriate antibiotic and replacement therapy as indicated. RESUME Les abces hypophysaires sont rares et demeurent tres difficile a diagnostiquer en pre-operatoire, malgre les nouvelles techniques d’imagerie medicale comme ie scanner et I’IRM. Nous decrivons 4 cas parmi lesquels 1 seul a ete diagnostique en pre-operatoire. Les abces hypophysaires peuvent avoir les memes signes cliniques qu’une meningite chez les patients ayant une selle turcique elargie a la radiographie cranienne. Il est generalement tres difficile de differencier a , l’examen clinique et radiologique, les abces des tumeurs hypophysaires. Le diagnostic est souvent pose au cours de l’intervention chirurgicale. Le traitement consiste en un drainage transsphenoidal, une antibiotherapie appropriee, et une therapeutique de substitution selon le besoin. Keywords : Pituitary abscess, pituitary infection, transsphenoidal drainage, Africa INTRODUCTION Pituitary abscess is an uncommon condition, even in an environment where intra-and extracranial sepsis is common. Since Simmonds published the first case of a pituitary abscess in 1914 [17] over 60 cases have been described. MATERIALS AND METHODS The Department of Neurosurgery at Groote Schuur Hospital managed 4 patients with this diagnosis between 1979 and 1995 and during the same period operated on 496 pituitary adenomas. Hospital records and neuroradiological reports were the sources of information about the cases presented here. Case 1 This 21 year old male presented in 1979 with 1 month’s history of headache which had become generalized and was unassociated with photophobia. As a child he was injured with a sharp object over the bridge of his nose. Six months prior to presentation he hit his head against the windscreen in a motor vehicle accident and may have had rhinorrhoea for about a week. He suffered intermittent headache from that time. On examination he was confused, drowsy and had neck stiffness but was apyrexial and his ears were normal. No abnormality was found on systemic examination and the cranial nerves and peripheral nervous system were intact. Haematological examination revealed a haemoglobin of lOg/dl, white cell count of 8000 and ESR of 60. A lumbar puncture yielded CSF at a pressure of 50 cm of water and was clear and colourless. Laboratory analysis of the CSF revealed: protein 5g/dl, globulin l+, glucose 2,5, polymorphs 87 and lymphocytes 97. Gram’s stain was, however, negative and there were no yeast’s on Indian ink staining. A remarkably enlarged sella with a thin dorsum sellae and opacification of the posterior part of the sphenoid sinus was shown on skull-xray. Tomography confirmed the sellar enlargement but CT scan showed no abnormality apart from this. Lumbar air encephalogram demonstrated a soft: tissue mass involving the sphenoid sinus, pituitary fossa and suprasellar region. On carotid angiography displacement of the A I segment upwards and the siphon laterally, but no tumour blush, could be seen. Because the patient presented with a sterile meningitis in association with an enlarged pituitary fossa and evidence of a soft tissue mass involving the sphenoid sinus and pituitary fossa region, the diagnosis of an infective lesion was made but no aetiological factor could be implicated.
At transsphenoidal exploration the sphenoid sinus was found to be occupied by yellowish chronic granulation tissue so that a craniopharyngioma was also suggested. Sinus aspiration yielded nothing but when the needle was advanced into the pituitary fossa, 4 ml of thick pus was obtained. The entire cavity was cleared of its purulent content, washed out with an antibiotic solution and using the image intensifier it was confirmed that the dome of the abscess had completely come down to the floor of the fossa. The post-operative course was unremarkable u2013 the only complication was a low serum sodium due to inappropriate ADH secretion. Case 2 This patient, a 76 year old man, had a background history of being treated for hypothyroidism and hypopituitarism for 11 years, and had been fully investigated for this 5 years prior to presentation. A lumbar air encephalogram showed no suprasellar extension of a pituitary mass at that stage and the lumbar CSF was normal. He presented to our department in 1982 with a history of severe headache and neck stiffness with episodes of reduction in his level of consciousness and a bilateral decrease in visual acuity for 4 months. He also had diplopia in all directions of gaze for 3 months. On examination no systemic abnormality was found. He was alert and fully conscious with no neck stiffness. The right pupil was slightly larger than the left but both were fully reactive. A decrease in visual acuity was noted and visual field tests revealed bitemporal hemianopia, fundi were normal. Full blood count, biochemistry, ESR and liver function tests were all normal. Tomography of the pituitary fossa suggested a non-invasive asymmetrical lesion within the fossa. CT scan identified a small isodense non-enhancing mass bulging upwards into the chiasmastic cistern but with no extension into the sphenoid sinus. At transsphenoidal exploration, the mucous membrane of the sphenoid sinus was found to be thickened, the sellar floor very thin, and on opening this, a copious volume of pus was drained. Culture of the pus showed no organisms and no acid fast bacilli were grown. He made an uneventful recovery and was soon back on his maintenance steroids. Case 3 A 24 year old female school teacher presented in 1990 with a years’s history of amenorrhoea, galactorrhoea, frontal headaches and increasing visual problems. Six months prior to referral to our department she was found to have an upper quadrantic bitemporal hemianopia and the prolactin levels were found to be mildly elevated. CT scan revealed a pituitary mass with suprasellar extension. 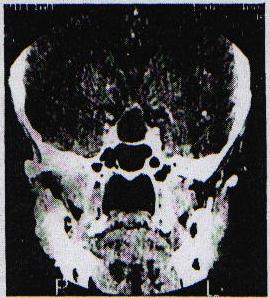 Figure 2 A prolactinoma was diagnosed and she was commenced on bromocriptine. There was, however, no improvement over the next six months, despite the fact that her prolactin was now in the normal range. There was no past history of note. Apart from bitemporal hemianopia, which was more extensive on the left, her clinical examination was non-contributory except for an ESR of 82 mm. At transsphenoidal exploration incision of the dura revealed pus. The cavity was adequately drained and the patient had an unremarkable post-operative course. The Gram’s stain revealed gram positive cocci but there was no growth on culture. On a follow-up CT scan in 1993 the abscess had, however, reformed. Clinically the patient was completely well and neurological examination, including the visual fields, was normal. As the patient was reluctant to undergo surgery she was placed on a 3 month course of antibiotic therapy. Follow up CT scan in 1994 revealed the abscess to be slightly larger, and it was re-evacuated transsphenoidally with a small drain left in situ for a few days to ensure complete drainage. She has subsequently made a good recovery and the abscess has not recurred on MRI scanning. Case 4 In 1992, this 41 year old male developed headaches and blurring of vision associated with severe thirst, polydipsia and polyuria. He also experienced sleep problems with snoring and excessive night sweats. His weight had increased and he had become impotent. On examination he was overweight, apyrexial with normal secondary sexual characteristics but hypogonadism was noted. Systemic examination and examination of the nervous system were normal with no papilloedema or visual field defect. Investigation revealed that his glucose tolerance test curve was impaired and the ESR was 32 mm. Endocrine testing revealed normal prolactin, thyroid hormone and FSH but testosterone was low. Testing of visual fields showed no evidence of chiasmal compression. On CT scanning a low density pituitary mass with slight suprasellar extension was demonstrated. MRI brain scan confirmed a mass lesion in the pituitary fossa with upward displacement of the optic chiasm. There was an area of enhancement with Gadolinium in the right upper aspect of the pituitary fossa. These features were brought to be in keeping with a pituitary macro-adenoma. 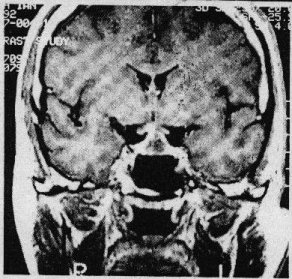 Figure 3 The patient was stabilized on Desmopressin preoperatively. On opening the dura at transsphenoidal exploration, pus was encountered. No pituitarys adenoma was found and after appropriate specimens for bacteriological assessment were taken, the abscess cavity was irrigated and closed. Staphylococcus Aureus was grown on culture and the appropriate antibiotic was commenced. The post operative course was uneventful. DISCUSSION The diagnosis of pituitary abscess remains a vexing clinical problem. It is rarely seen in acute phase by experienced practitioners so that a pre-operative diagnosis is hardly ever made and a surprise finding at surgery or autopsy is often the course of events. CLINICAL PRESENTATION No age or sex prevalence is evident in the world literature on this condition [1,3,10]. Symptoms usually develop over a few months but in a few cases very acute evolution has occurred [10]. The mass effect may cause headache and visual loss gradual loss of vision due to extension of the tumour above the level of the diaphragma sellae is usual, but may be as acute as in pituitary apoplexy [16]. Endocrine deficiency may or may not be present, depending on the duration of the disease and the degree of compression of the pituitary. The presentation of the pituitary abscess may, therefore, be distinguishable from that of a pituitary tumor 114]. Indeed, the abscess may develop within a primary pituitary tumor or cyst [16]. It has been stated, however, that the development of diabetes insipidus may help differentiate a pituitary abscess from a tumour. Diabetes insipidus only develops in 10% of pituitary adenomas but commonly occurs in the evolution of pituitary abscesses [9] and metastatic tumours of the pituitary. The presence ol combined anterior and posterior pituitary disturbance in the absence a hypothalamic lesion should also arouse the suspicion of an abscess [1]. Three of our patients presented with a combination of headache, visual disturbance and endocrine dsyfunction thought to be compatible with a pituitary adenoma. Significantly, the one patient had Diabetes insipidus as his presenting complaint. There may be associated meningitis and this feature in the presence of a large sella due to a known or suspected pituitary tumour should raise the possibility of this diagnosis [1,3,6,8). It has, however, been noted that less than half of the patients with a pituitary abscess will have a meningitic picture [3]. Sellar enlargement associated with pituitary failure and intermittent attacks of meningitis may, however, also be a feature of Rathk cleft cysts. On the other hand, there may be a remarkable absence of any meningitic reaction in the presence of a florid sellar abscess [14]. Our one patient presented with a meningitis following a skull base fracture and also had a large sclla on skull x-ray. The most common way a pituitary abscess presents is as a surprise finding at surgery [3]. AETIOLOGY A sellar abscess may follow previous surgical exploration [3] or Yttrium implantation and in the latter instance, aspergillosis is a particular common causal organism [7]. It may occur in a preexisting chromophobe pituitary adenoma 14,11,18,19] or a Rathke’s cleft cyst [12]. Dominique and Wilson [6] stated that pituitary tumors become susceptible to infection because of impaired circulation, areas of necrosis, or local immunological impairement. It may result from local extension of chronic sphenoid sinusitis, [3,19] but this is probably very rare.Our one patient (Case 1) developed a pituitary abscess following a probable basal skull fracture suggesting this as a possible post-traumatic complication. This patient as well as patient no. 2 had evidence of sphenoid sinus infection. In the past a pituitary abscess as a feature of a septicaemic state was noted [8,17], but this has become extremely rare. Most commonly it seems to arise spontaneously. MICROBIOLOGY Gram’s stain was done on all specimens which showed the typical features of pus. Staphylococcus Aureus was cultured from case 4 and the other three cultures were negative although gram positive cocci were seen in case 3. The organisms are almost always bacterial, although the occasional fungal abscess has been reported [14] and this has been particularly so in patients who had. Yttrium implantations, probably due to the immuno-compromised state of the patient [6]. In more than half the reported cases no organism was cultured, but anaerobic organisms were not always looked for [1,8,11,16]. In addition the finding of sterile pus may also be due to the use of antibiotics prior to surgery. Organisms identified are unremarkable but may be of low virulence or usually non pathogenic [10,16]. DIAGNOSIS Diagnosis is difficult pre-operatively as there may be very little to suggest an infective process. One of our patients had a normal sedimentation rate and only one was febrile. CSF analysis may be abnormal although not invariably so [14] and is not frequently done. Plain radiology of the skull always shows an enlarged sella turcica [2,3,8,9]. The fact that the sella is enlarged indicates some chronicity of this lesion and if associated with pituitary failure, implies that the process has been present for a considerable time. A variety of CT scan have been described with pituitary abscess. A low density intrasellar mass with a cystic appearance and marginal contrast enhancement are almost always demonstrated, but these features are not specific to pituitary abscess. We have encountered them in a infarctive pituitary apoplexy [5]. Features that may be more specific are permeative destruction of the sella floor, heterogenecity of the cyst contents suggesting the presence of debris in the cyst and cystic dilatation of the infundibulum [1]. CT scans in apost-surgical patient are particularly difficult to interpret in the diagnosis of an abscess [6]. MRI scan performed in one of our patients showed an area of enhancement compatible with a microadenoma. MRI has been found to be superior to CT scan in 41 % and equal in 54% of cases of sellar and parasellar masses [9], but has not as yet been proved to be a better diagnostic tool for the diagnosis of a pituitary abscess. TREATMENT In a patient presenting with meningitis and an enlarged fossa which suggest the diagnosis, prompt treatment with antibiotics should follow. If this does not result in immediate improvement, the sella should be explored and the abscess drained transsphenoidally. This route allows drainage without risk of contaminating the subarachnoid space [6,11,19]. PROGNOSIS Robinson has stated that the major cause of poor prognosis is delay in diagnosis and surgical treatment [15]. Pituitary abscess has an overall mortality of 28%, however those patients with meningitis have poorer outcome with a mortality of 45% [6]. CONCLUSION Pituitary abscess is a rare but potentially fatal condition. It may present as a meningitic illness or as a sellar mass lesion with endocrine and visual abnormalities. There is an enlarged sella on skull x-ray and cystic mass lesion on CT scan or MRI. Prompt treatment with antibiotics, steroids and transsphenoidal drainage should ensure good recovery for the patient. The majority of pituitary abscesses will, however, probably still be a surprise finding at surgery.
SUMMARY A retrospective study on 213 files of epileptic patients issued from a sample of 741 referrals to the University Hospital ofMajunga, Neuropsychiatry Unit, between June 1, 1993 December, 31, 1995 was reported. RESUME Une etude retrospective des dossiers de 213 epiletiques tires d’une population de 741 malades admis au niveau d’un service de Neuropsychiatrie de Mahajanga (du 01.06.93 au 31.12.95) est rapportee. Cette ville, chef-lieu de la province du meme nom a un climat et sec ou Ie paludisme, la bilharziose, la tuberculose et la syphilis sont endemiques. Comme dans la plupart des series tropicales, la tranche d’age la plus atteint est celle comprise entre 10 et 30 ans; les crises partielles predominent sur les formes generalisees (52% vs 46%). Les facteurs de risque les plus importants sont d’origine parasitaire (neurocysticercose) ou lies aux conditions obstetricales (souffrances perinatales) et pediatriques precaires (convulsions febriles). Keywords : Epidemiology, Epilepsy, Madagascar, Africa INTRODUCTION In a recent Press release (1), the World Health Organisation (WHO) launched, jointly with two non-governmental organisations (the International League Agaisnt Epilepsy, ILAE, and the International Bureau for Epilepsy, IBE), a worldwide campaign against epilepsy. The ILAE represents doctors and scientists, whereas the Bureau acts for patients and their families. Anyhow, three-quarters of the affected people (up to 30 millions, 90% of whom are in developing countries) do not receive any treatment at all, and must be brought out of the shadows (1). In Madagascar, a tropical Island in the Indian Ocean, no epidemiological data from the general population is available. In the present hospital-based study, we report some aspects of epilepsy from the Northwestern part of the island. MATERIALS AND METHOD The study took place in the only Department of Neurospsychiatry, expected to serve the whole province of Mahajanga (1,379,000 inhabitants). In fact, geographical isolation (seasonal roads), economic restraints, preference for traditional healers and sometimes pure fatalism, limited the access of the Department to the only inhabitants of Mahajanga City and its nearest surroundings. The province has a dry and hot climate, where malaria, schistosomiasis, tuberculosis and syphilis are endemic. The study population (3) was young (44% of the people were less than 15 years-old, only 3.20% were 65 years-old or more), and had a low instruction level (table 1). Table 1: Comparative instruction level of patients versus that of the general population.
Ethnical groups distribution is plotted on table 2. Certain ethnics (Comorois, Sakalava…) have a strong Islamic influence. Table 2: Comparative distribution of different ethnical groups (in %), between epileptic patients and the population of MAHAJANGA City.
The study itself consisted in a retrospective review of patients’ files. Neurological patients of 1 year-old or more, who have been attending the Department, between June 1, 1993 and December 31,1995, were included. Basic neurodiagnosis facilities (EEG, EMG, brain imageries) were lacking, so case ascertainment-were set up only with clinical criteria, routine laboratory exams and therapeutic tests. We used the International Classification of seizures, ICES, 1981 version (4) without EEG data, recognised by some authorities (5). Term definitions were extracted from the guidelines of the ILAE (5)]: febrile seizures, single or isolate seizures were thus excluded. RESULTS The epilepsies 0^=213) represented 28.75% of all new neurological referrals (n=741) for the period (table 3). Table 3: Aetiological repartition of neurological referrals (in percentage) during the study period.
It was possible to classify 98% (208/213) of the seizures (table 4). Table 4: Comparative patterns of epilepsies between series from developed countries.
The mean age of the patients was 23.96 years with a dispersion varying between 1 year and 73 years. More than 1 patient out of 2 were less than 20 years-old (table 5). Table 5: Age distribution of epileptic patients (in percentage).
Assumed secondary epilepsies supervened significally later than primary ones Mean age of occurrence respectively 30.56 years and 17.36 years). There was male predominance (sex ratio=l 27/86=1.48). Certain ethnical groups (Merina, Betsileo) were over represented (table 1). Forty two per cent (42%) of the patients (90/213) were students, 36% were unemployed (77/213). Farmers represented only 6,8% of care-attenders (14/213); it confirms the preferential recruitment of urban city dwellers. Epileptic patients had a significantly higher level of instruction, compared to the general population (table 1). Eighty per cent (80%) of cases (170/213) had at least one crisis per year. Partial seizures accounted for 52% of cases (111/213); among them, the simple type was prevalent (table 4). Table 6: Likely aetiologies of secondary epilepsies, referred to partial and all types of seizures.
Sixteen per cent (165%) of the patients (34/213) had a previous history of febrile convulsion, 13% of them (28/213) had a minor or specific cerebral dsyfunctions and 5.5% (12/213) had a mental retardation. The physician rarely witnessed an attack, so the clinical disgnosis of epilepsy was essentially anamnestic. In regard to « Grand Mal» seizure, ten criteria were used to identify it in rural area surveys in Africa, Asia, and South America (6). The basic sign was the loss of consciousness for 1 to 30 mn:, only 15% of our crisis attenders were able to give the right duration of the seizures. The second major criteria was the sequence of a tonic, then a clonic phase of movements: here again, only 25% of witnesses could describe it accurately. We find it more informative to make people mimick crisis. Foaming at the mouth was reported in 80% of cases, but it was also observed in some hysterical attacks. Lateral tongue biting (57%), sphincter disturbances (47%) and fall stigma (40%) are more specific but in our observations they were not very sensitive. Phenobarbital (PB) was prescribed in 83.50% of cases (178 prescriptions out of 213), and was generally well tolerated (in 85% of patients). Carbamazepine (7.50% of prescriptions) exposed to further treatment gap, because of its high cost and its bad distribution. The effect of the treatment was good; 55% of the patients (118/213) had 50% of their seizures controlled; yet, long term follow-up was uncertain. DISCUSSION Our hospital-based study is not designed to assess morbidity rates (incidence, prevalence), because of selection biases. CONCLUSION The global campaign launched by the WHO against epilepsy, expresses the importance of this disease. This stigmatizing illness constitute a real Public Health problem for the Third World. SUMMARY A prospective study of all head injured patients who were admitted to the Parirewyatwa Hospital under our care between the months of May 1996 and August, 1997 inclusive was undertaken. The purpose of the study was to document the cause and nature of the injury, the presence of other injuries and their effects, the outcome, to review the post mortem in order to clearly delineate the nature of the intracranial injury, to determine if there were errors in the treatment, to see if there were other ways in which the treatment of the head injuries could be improved. RESUME Une etude prospective a ete conduite chez tous les patients ayant presente un traumatisme cranien, admis dans notre service a 1’Hopital Parirewyatwa entre les mois de Mai 1996 et d’Aout 1997 inclus. Le but de 1’etude etait de rechercher les causes et la nature du traumatisme, la presence d’autres blessures et leurs effects, leur devenir. De plus, les rapports d’autopsies ont ete examines pour rechercher la nature exacte des lesions intracraniennes afin de determiner s’il y avait eu une erreur dans le traitement, et pour rechercher s’il etait possible d’ameliorer les therapeutiques des traumatismes craniens. Keywords : Head injuries, Critical Review, Treatment, Africa 1. The cause of and nature of the injury. Table 1
Road traffic accidents constitued the major incidence. (Table 2): Table 2
Admission policy at the Parireyatwa Hospital decrees that head injuries take priority so that a considerable number of patients with other injuries as well as those of the head are brought into our ward. (Table 3): Table 3
These figures are not strictly comparable except to suggest that the chances of dying are slightly greater for those with other injuries that with a head injury only, and for those with a head injury it is just over 10% understandably multiple injuries were commonest in the R.T.A. Group. The patients were classified according to their Glasgow coma scores which were estimated soon after admission to the ward or Casualty Department and it was frequently impossible to determine exactly how long, post injury this was, patients transferred frrom outside the town had the Coma Score assessed by the referring doctor before their departure. The coma score was measured out of 14 and the patients were divided into three groups on that basis. (Table 4): Table 4
As would be expected the mortality was highest in the low coma score and lowest in the high coma score groups. 50 patients died overall. 36 of these were the subject of post mortem examination and 5 others had a clear definition of their intracranial status by CT Scanning. Nine patients had neither CT Scan nor autopsy but seven of these had been admitted deeply unconscious and died 48 hours without improvement, so I think we have a fair idea what was going out there. In group I, where 35 out of 75 patients died, there were three interesting cases:- The patients had normal scans yet they died after four and 21 days, in the third case at autopsy there was only subarachnoid heamorrhage and a very small subdural blood collection and it was difficult to see why these three patients died. In group II where 10 out of 79 patients died one showed a mild diffuse brain swelling but nothing else, while a second showed small occipital haemorrhage, a small subdural haemorrhage and extensive cerebral oedema. Another patient showed a severe bronchopneumonia with only minor brain change. A fourth patient, a 25 year old male suffered a fractured tibia and fibula as well as a head injury, his conscious level dropped from 14/4 to 9/14 after reduction of the fracture. A Clinical diagnosis of fat embolism was made – post mortem examination confirmed the diagnosis. Five patients out of 217 died in group III (2.2%) and in some ways these are the most interesting COMMENTS Three problems seem to arise from this: (1) Epidural haematoma, provided it follows the classical pattern is very curable if intervention occurs in time. How can this be facilitated? It is clear that simple clinical observation is inadequate in some cases, where there is easy access to a CT Scanner there should be no problem but where there is not some easier and cheaper method must be employed. Early Angiography is one possibly but it needs a reasonable set up and it is invasive. Basically what is needed is a non invasive, non damaging, easily applied test will show the position of the midline of the brain relative to the centre of the skull – where the midline is centrally placed we can be sure there is no surgical lesion. 1 am suggesting that we try to revamp ultrasound scanning which proved it- self most valuable in the past. There was an instrument called the « Midline » which anyone could use and which could accurately locate the midline structures without difficulty or danger. We used it for many years – unfortunately no one in the northern hemispheres makes it now – though I have tried hard to get one made no one will do so because the first world does not want it. I believe that a cheap reliable model could help us tremendously in the third world. One of these machines in each District Hospital could help the resident doctor to decide whether urgent transfer is necessary. (2) The second point reveals a different aspect of head injury care – that of care of the airway. When I first came into neurosurgery the importance of airway clearance was not appreciated and I have seen patient literally roaring with laryngeal spasm and tracheal mucous. We eventually got the idea that this had to be removed and started to bronchoscope the patients. We then went over to tracheostomy with very gratifying results and later to endotracheal tubing with what I believe, have been less successful results. In a number of the cases reported here there was evidence of inadequate airway clearance. The patient with cardiac tamponade was a surprise. (3) In six cases the brain injury appeared minimal and at CT Scanning or autopsy various authors have pointed out how trauma, and particular bruising or the brain with haematoma formation and neuron distracted liberates toxic cytokines as well as electrolytes in the extra cellular fluids with resulting brain swelling and dsyfunction. There were more of these cases than those requiring surgery. This means that while we must tighten up on our diagnosis and observations and on our general and especially airways care, it also means that the main focus of our attention has to be on the development of techniques to mitigate the deleterious effects of these liberated substances that has to be the main thrust of head injury research now. CRANIOPLASTY WITH INNER TABLE OF BONE FLAP IN CHILDREN: REPORT OF TWO CASESSummary Cranioplasty is performed with various materials and autogenous bone. Since 1956 the Author has adopted the cranioplasty with acrilic resin in 149 consecutive cases and is satisfied with this technique in adult patients, less so in children where, due to the growing of the head and growing of the bone around the skull defect the acrilic cranioplasty can be displaced with bad cosmetic results so much that often it requires redoing. For this reasons the Author has adopted recently the cranioplasty with inner table of bone flap as described by KAZUHIKO et all in 1985. This technique has been used to repair the skull defect in two children with very satisfactory results. It is worth reporting this method of grafting applicable in various situations. particularly in children and especially in Africa where acrilic resin may not be available. Resume Les cranioplasties sont effectuees avec differents materiaux et avec de 1’os autogenique. Depuis 1956. I’auteur a utilise dans 149 cas la resine acrylique avec satisfaction chez les adultcs. Chez les enfants, par contre, en raison de la croissane du crane, la cranioplastie acrylique peut se deplacer, de telle sorte qu’il faut souvent la refaire. C’est pourquoi l’auteur a recemment utilise la table interne de 1’os comme lambeau, selon la technique decrite par KAZUHIKO et al en 1985. Elle a ete utilisee chez deux enfants avec d’excellents resultats. En outre, ce type de greffe peut etre utilise dans differents cas chez les enfants, tout particulierement en Afrique ou la resine acrylique n’est pas toujours disponible. Keywords : Cranioplasty, autogenous bone, children, Africa The cranioplasty is performed with autogenous bone and other materials. Whilst the autogenous bone graft is more physiological, it has various inconveniences mainly in the repair of large skull defects, the donor place (tibia, ribs, scapula and iliac bone) that results at the end cause of more problems that the actual cranioplasty, is more traumatizing, time consuming, prolonged hospitalization. In the last decades the preference has been given to the cranioplasty with acrilic resin that has the following advantages: is a simple technique not requiring long time to perform, possibility of modelling perfectly and insert directly the cranioplasty using as mould the skull defect, good tissue tolerance. The material is insulating, avoid the inconveniences of heating, is radiotransluccnt, docs not modify the EEG. low cost compared with other materials, possibility to perform in any moment without any special preparation, a cranioplasty with good cosmetic results of any skull defect, large or small or irregular. These are the reasons why since 1956 the cranioplasty with acrilic resin has been performed by the Author in 149 consecutive cases. CASE 1 This 6 year old female was hit on the head in Rwanda in May. 1994. Had a depressed skull fracture and the depressed bone was removed by a local surgeon. She had a circular bone defect of the diameter of 5 cm in the right occipital region, well pulsating. No neurological deficits. On the 22nd November. 1995 a large bone dowel was taken in the parietal area and the bone was splitted with a chisel. Replacement of the cortical bone at the donor site and placement of the inner table at the level of the skull defect. Both bone flaps were Fixed with chromic catgut. Closure in layers over suction drain. The post operative course was uneventful. Cosmetic results excellent. The postoperative x-rays some months later showed good results of grafting. CASE 2 This 8 year old male was hit in the right parietal region in May, 1994 in Rwanda. Had a depressed skull fracture with a mild left hemiparesis. On the 29th November, 1995 the depressed skull was removed. A bone flap was performed in the right occipital area and the inner table ciseled out to repair the bone defect. Replacement of the cortical bone flap in the donor place and fixing of both bone flaps with chromic catgut. Closure in layers over suction drain. The post operative course was uneventful. The post operative x-rays six months later showed a good result of the grafting. DISCUSSION Despite the autogenous bone is the most suitable material for cranioplasty because of its anatomical similarity to the skull, the use of the standard acrilic cranioplasty remains at present the procedure used by most neurosurgeons. This is mainly due to the fact that the bone is rigid and it can be difficult to contour the graft with respect to skull defect, surgery and possibility of infection and pain at the door site, time consuming and other reasons that have made the autogenous bone for cranioplasty less and less popular. On the other hand, in children the use of standard acrilic cranioplasty has some disadvantages due to the growing of the child’s head with possibility of displacement of the cranioplasty with bad cosmetic results. This was the reason while in this two children we have used the technique described by KAZUHIKO et all in 1985 with satisfactory results. Articles récents
Commentaires récents
Archives
CatégoriesMéta |
© 2002-2018 African Journal of Neurological Sciences.
All rights reserved. Terms of use.
Tous droits réservés. Termes d'Utilisation.
ISSN: 1992-2647



